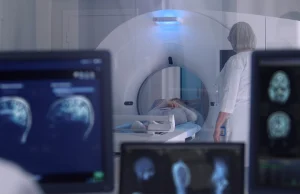
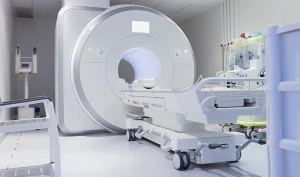
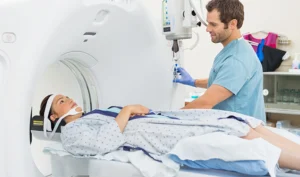
Every seven minutes, someone in America receives a lung cancer diagnosis. By the time symptoms appear – persistent cough, unexplained weight loss, shortness of breath – the disease has often progressed beyond its most treatable stages. The preventive imaging industry observes this pattern repeatedly, and the data reveals a troubling truth: many of these cases could be detected years earlier with a 10-minute lung scan costing less than most monthly car payments.
The economics of lung cancer screening present a striking contradiction. People spend hundreds monthly on car insurance they hope never to use, yet hesitate at a one-time scan that could save their lives. Understanding the actual costs, benefits, and limitations of lung screening helps you make informed decisions about this potentially life-saving investment.
What You Need to Know About Lung Scan Costs and Benefits
- Actual price ranges: Lung CT scans cost $150-$500, making them among the most affordable preventive screenings available
- Detection capabilities: Low-dose CT scans identify lung nodules as small as 3mm – years before symptoms develop
- Survival rate differences: Early-stage lung cancer shows 80-90% five-year survival versus 6% for late-stage diagnosis
- Radiation exposure reality: Modern low-dose protocols deliver radiation equivalent to six months of natural background exposure
- Insurance coverage availability: Medicare and most insurers cover annual screening for high-risk individuals meeting specific criteria
The value proposition extends beyond immediate cost considerations. Late detection transforms a potentially manageable condition into a life-threatening crisis with treatment costs reaching hundreds of thousands of dollars. Early detection through affordable screening offers intervention when treatment works best and costs least.
Understanding Lung Scan Technology and Price Variations
Not all lung scans deliver equal value – and understanding the differences directly impacts both cost and health outcomes. The gold standard for lung cancer screening is low-dose CT (LDCT) scanning, technology that produces detailed images while minimizing radiation exposure.
Cost variations by provider type:
- Standalone screening centers: $150-$300 for basic LDCT without additional facility fees
- Hospital radiology departments: $300-$800 including higher facility fees and administrative costs
- Preventive health centers: $200-$500 typically including board-certified radiologist interpretation
- Mobile screening units: $99-$199 during promotional events, though may use older equipment
- Package combinations: Often bundled with heart scans for $250-$400 total, providing better per-scan value
Price differences reflect more than overhead – they include technology quality, radiologist expertise level, report comprehensiveness, and follow-up support availability. A $99 promotional scan might use older equipment or provide minimal interpretation, while higher-priced options offer detailed analysis and consultation explaining findings in clear language.
What affects image quality and detection accuracy:
Equipment age matters significantly. Scanners from the last five years provide superior image quality at lower radiation doses than older models. Facilities should use CT scanners with at least 16 detector rows – newer 64-slice or higher systems offer even better resolution.
Radiologist specialization impacts interpretation quality. Board-certified radiologists with subspecialty training in chest imaging catch subtle abnormalities that general radiologists might miss. Ask about interpreter qualifications before booking.
Who Should Consider Lung Screening Beyond Official Guidelines
Official screening guidelines target specific high-risk groups, but lung cancer risk extends beyond these neat categories. Traditional screening criteria focus on adults 50-80 years old with 20+ pack-year smoking history who currently smoke or quit within 15 years.
Guidelines miss several important risk groups:
- Never-smokers with significant secondhand exposure: Living or working with smokers for decades increases risk substantially
- Family history carriers: First-degree relatives with lung cancer elevate your risk regardless of smoking status
- Occupational exposure workers: Asbestos, radon, diesel exhaust, silica dust, and other carcinogens increase lung cancer risk
- Radiation therapy recipients: Previous chest radiation for other cancers creates elevated lung cancer risk
- Chronic lung condition patients: COPD, pulmonary fibrosis, and other conditions increase cancer probability
- Light smokers below pack-year thresholds: 10-15 pack-year histories still carry meaningful risk
The question becomes whether a few hundred dollars for knowledge about your lung health makes sense given your specific risk factors – even if you don’t meet official screening criteria.
The Financial Reality of Late Detection
Comparing preventive scan costs against late detection expenses reveals dramatic differences. Early-stage lung cancer treatment ranges from $50,000-$75,000 with excellent survival outcomes. Late-stage treatment? Expect $200,000-$500,000 with dramatically reduced survival probability.
Hidden costs of late detection extend beyond medical bills:
- Lost income during treatment: Average 12-18 months away from work during intensive therapy
- Caregiver opportunity costs: Family members often reduce work hours significantly or leave jobs entirely
- Travel and relocation expenses: Specialized treatment centers may require temporary or permanent moves
- Home modification costs: Oxygen equipment, mobility aids, safety updates, and accessibility changes
- Psychological and quality of life impacts: Depression, anxiety, relationship stress, and reduced life satisfaction
- End-of-life care expenses: Palliative care, hospice services, and final arrangements
A $300 preventive scan transforms from expense into insurance with actual utility – coverage you can use before problems develop rather than after.
What Lung Scans Detect and Their Limitations
Modern LDCT scans excel at finding abnormalities that chest X-rays miss entirely. Detection capabilities include:
- Lung nodules: Small growths as tiny as 3 millimeters become visible
- Ground-glass opacities: Hazy areas that may represent early-stage cancer
- Emphysema and COPD changes: Structural lung damage from smoking or other causes
- Coronary artery calcification: Bonus cardiovascular information from the same scan
- Other chest abnormalities: Infections, inflammation, structural issues, and incidental findings
Important limitations to understand:
Lung scans cannot determine whether nodules are cancerous without additional testing. They detect structural changes but require follow-up procedures for definitive diagnosis. They don’t catch all lung cancer types with equal accuracy – some aggressive forms grow between annual screenings.
Scans cannot predict future cancer development or guarantee you won’t develop lung cancer after a clear result. They represent a snapshot of current lung status, not a permanent all-clear signal. Finally, they don’t replace the need for follow-up care – detected abnormalities require appropriate monitoring or intervention.
Understanding these limitations sets realistic expectations while appreciating the technology’s genuine life-saving capabilities.
Addressing Radiation Exposure Concerns
Radiation exposure represents the most common concern among potential screening candidates. The question deserves honest, contextualized answers.
Radiation dose comparison in millisieverts:
- Low-dose lung CT scan: 1.5 millisieverts
- Annual natural background radiation: 3 millisieverts
- Cross-country airline flight: 0.03 millisieverts
- Standard chest X-ray: 0.1 millisieverts
- Conventional CT scan: 7 millisieverts
- Cardiac stress test with imaging: 10-15 millisieverts
One LDCT scan delivers radiation equivalent to approximately six months of normal environmental exposure. Comparing this minimal risk against the substantial risk of missing early-stage lung cancer clarifies the risk-benefit equation.
Modern protocols continue reducing radiation doses while maintaining or improving image quality. Current scanners deliver significantly lower radiation than equipment from even five years ago. The technology literally becomes safer while becoming more effective.
For appropriate-risk individuals, radiation concerns shouldn’t prevent screening. The cancer detection benefit far outweighs the minimal radiation risk from low-dose protocols.
Insurance Coverage: When Screening Costs Nothing
The Affordable Care Act mandates coverage for lung cancer screening in high-risk individuals who meet specific criteria. When you qualify, scans cost nothing beyond potential copays or deductibles.
Coverage specifics by insurance type:
- Medicare Part B: Full coverage for eligible beneficiaries including required counseling visit with ordering physician
- Private insurance plans: Most plans cover with no cost-sharing for individuals meeting screening criteria
- Medicaid programs: Coverage varies by state but generally includes screening for high-risk groups
- Employer health plans: Often include preventive screening benefits beyond minimum ACA requirements
- Veterans Affairs: Covers eligible veterans meeting standard screening criteria
The qualification catch:
Meeting one criterion isn’t enough – you must satisfy all requirements and follow proper procedures. Missing documentation, incorrect coding, or procedural errors mean paying full price. Work with your ordering physician to verify eligibility and proper authorization before scheduling.
Some facilities require pre-authorization while others handle this administratively. Clarify financial responsibility upfront to avoid surprise bills.
The Screening Follow-Up Process and Additional Costs
Finding something on your lung scan doesn’t equal cancer diagnosis. Most detected nodules prove benign, but each requires appropriate follow-up based on size, appearance, and growth patterns.
Typical follow-up pathways by finding type:
- Benign-appearing nodules: Annual surveillance scans to confirm stability over time
- Indeterminate nodules: Follow-up imaging in 3-6 months to assess for growth or changes
- Suspicious findings: Additional testing including PET scans, bronchoscopy, or biopsy procedures
- Clearly malignant appearances: Immediate referral to thoracic surgery or oncology
This follow-up process adds potential costs but provides crucial benefits including active monitoring for changes, early intervention if abnormalities progress, baseline comparisons for future imaging, and detection of incidental findings that might matter for other health conditions.
Follow-up imaging often qualifies for insurance coverage since it investigates specific findings rather than providing general screening. This shifts many subsequent costs from out-of-pocket to covered services.
Making Your Personal Investment Decision
The decision to invest in lung screening ultimately depends on personal risk assessment and individual circumstances. Consider these factors in your evaluation:
- Your specific risk profile: Smoking history duration and intensity, occupational exposures, family history patterns, current age
- Financial capacity: Can you afford the scan without creating financial hardship or sacrificing essential expenses?
- Psychological response to uncertainty: Will knowing results (or not knowing) create more anxiety than reassurance?
- Follow-through commitment: Will you pursue recommended follow-up testing and monitoring if abnormalities appear?
- Health management philosophy: Do you prioritize prevention and early detection over reactive treatment approaches?
- Insurance qualification status: Do you meet criteria for covered screening or face out-of-pocket payment?
For many people, spending a few hundred dollars for potentially life-saving information represents worthwhile investment. For others, uncertainty about findings creates more distress than benefit. Neither choice is inherently wrong – but make the decision consciously rather than through inaction.
Maximizing Value from Your Lung Scan Investment
If you decide to proceed with lung screening, maximize your investment through informed provider selection:
Prioritize quality over lowest price:
- Board-certified radiologist interpretation with chest imaging subspecialty training
- Modern equipment using current low-dose protocols
- Detailed written reports explaining findings in understandable language
- Access to follow-up consultation for questions about results
- Clear communication processes for delivering results
- Established pathways for additional testing if needed
Consider combination packages for better value:
Many screening centers offer packages combining lung scans with other imaging:
- Lung plus heart scan combinations
- Full-body scans including detailed lung imaging
- Annual screening memberships with discounted rates
- Family or group discount programs
Strategic timing can reduce costs:
- End-of-year FSA/HSA fund usage before expiration
- Lung Cancer Awareness Month (November) promotional periods
- New screening center openings with introductory pricing
- Community health screening events with volume discounts
Craft Body Scan offers lung screening with board-certified radiologist interpretation using modern low-dose CT protocols. Their transparent pricing includes complete reports and consultation explaining findings. Package options combine lung screening with heart and other scans for better value while their team helps determine if you meet insurance coverage criteria.
Why Early Detection Creates Better Outcomes
Statistics tell part of the story, but real-world outcome differences drive the point home. Early detection through screening enables:
- Minimally invasive procedures: Small tumors often removable through limited surgery
- Better lung function preservation: Less tissue removal means better breathing capacity
- Faster recovery periods: Smaller surgeries require shorter hospital stays and healing times
- Higher quality of life: Less aggressive treatment causes fewer side effects and complications
- Dramatically improved survival rates: 80-90% five-year survival for early-stage versus 6% for late-stage
Late detection typically results in:
- Extensive or inoperable tumors: Advanced cancer may spread beyond surgical treatment options
- Aggressive chemotherapy and radiation: Intensive treatment protocols with significant side effects
- Substantial lung function loss: Large tissue removal or radiation damage reduces breathing capacity
- Extended treatment periods: Months or years of ongoing therapy
- Limited treatment options: Advanced disease restricts available interventions
- Poor survival probability: Late-stage diagnosis carries grim statistical outcomes
The contrast between these scenarios couldn’t be starker or more motivating for those weighing screening decisions.
Taking Control of Your Lung Health
The question isn’t whether lung scans provide value – evidence clearly demonstrates they do for appropriate-risk individuals. The real question is whether you prioritize prevention and early detection enough to invest in screening before symptoms force your hand.
Modern lung scans represent medicine’s most cost-effective cancer screening technology: affordable imaging capable of detecting cancer when it’s most treatable. Whether you qualify for covered screening or choose to pay out-of-pocket, the investment in knowledge about your lung health pays dividends in reassurance and potentially saved lives.
Don’t wait for symptoms to eliminate your choice. Don’t let cost concerns override health priorities when we’re discussing potentially life-saving screening. If you’re considering lung screening, research your options thoroughly, understand both benefits and limitations, and make informed decisions.
When it comes to lung cancer, early detection doesn’t just reduce expenses – it saves lives. That return on investment exceeds anything financial advisors can offer.
Schedule your lung scan at Craft Body Scan and invest in early detection that could save your life.