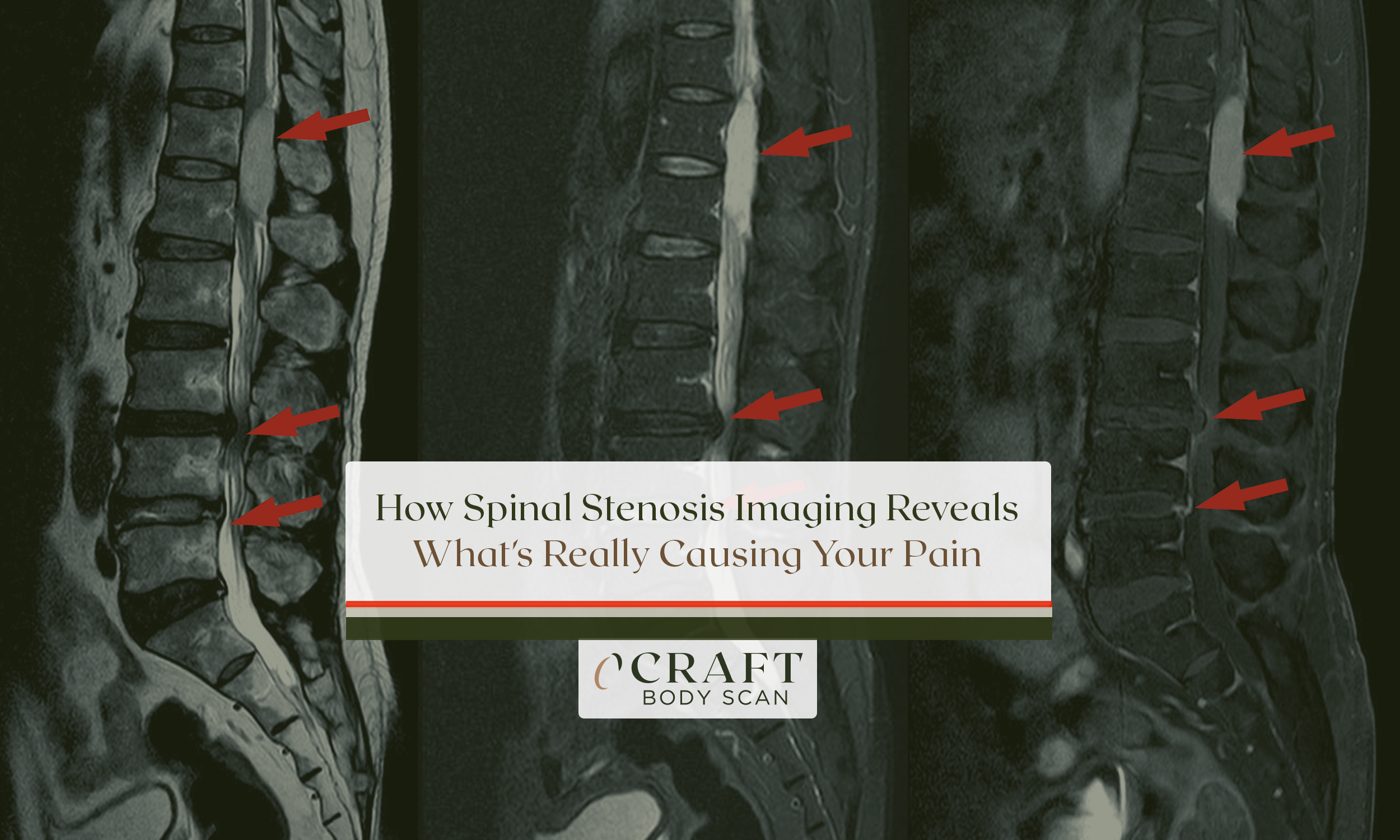
A spinal stenosis MRI is the standard imaging test doctors use to evaluate narrowing of the spinal canal. The scan shows the canal, discs, ligaments, and nerve roots together in a single exam, making it possible to measure how much space remains and whether the nerves or spinal cord are under pressure. Unlike X-rays, which only show bone structure, full body MRI and CT scans reveal the soft tissue changes that cause symptoms like leg pain, numbness, and difficulty walking.
If you have been ordered an MRI for spinal stenosis or have received results you are trying to understand, this guide explains what the images show, how radiologists measure severity, and how those findings connect to treatment decisions.
What Does a Spinal Stenosis MRI Show

In a spinal stenosis MRI, radiologists look at every structure surrounding the spinal canal and measure how much it has narrowed. The scan is detailed enough to distinguish the spinal cord, individual nerve roots, the fluid surrounding them, the discs pressing from the front, and the ligaments thickening from the back, all in the same image.
A healthy spinal canal shows a clear ring of bright cerebrospinal fluid surrounding the nerve bundle on T2-weighted sequences. As stenosis develops, that ring narrows. At the most advanced grades, it disappears entirely.
The findings radiologists document on a spinal stenosis MRI typically fall into these categories:
- Narrowed spinal canal - reduced space measured in millimeters or as a cross-sectional area in square millimeters at the most compressed level
- Compressed nerve roots - individual nerves that appear crowded together rather than separated by visible fluid
- Bulging or herniated discs - disc material pressing toward the canal from the front, visible as a dark protrusion on the bright fluid background
- Thickened ligamentum flavum - the posterior spinal ligament appears as a dark band encroaching from the back of the canal
- Facet joint arthritis - enlarged joints contributing to canal narrowing from the sides
- Bone spurs (osteophytes) - bony growths at vertebral margins where the spine has attempted to stabilize degenerating segments
- Reduced cerebrospinal fluid space - the clearest visual indicator of stenosis grade on any spine MRI
- Spinal cord signal changes - bright areas within the cord itself, seen in cervical cases where compression has been sustained long enough to affect cord tissue
Radiologists use standardized grading systems to ensure consistent interpretation. The Lee grading system classifies central canal stenosis from Grade 0 (normal) through Grade 3 (severe), based on the degree of cerebrospinal fluid obliteration around the nerve bundle.
Why MRI Is the Best Imaging Test for Spinal Stenosis
MRI has become the preferred first choice for evaluating spinal stenosis because it shows both the bony canal and the soft tissue structures that narrow it, without radiation. That combination is not available with any other imaging modality.
X-rays show bone alignment but cannot visualize discs, ligaments, or nerves. CT scanning provides superior bone detail but does not show soft tissue with the same clarity. The Mayo Clinic identifies MRI as the primary diagnostic tool for spinal stenosis because of this advantage over other modalities.
MRI also produces images in multiple planes and with multiple tissue contrasts in a single session. T1-weighted sequences show anatomy and fat signal clearly. T2-weighted sequences make fluid appear bright, so any reduction in cerebrospinal fluid around the nerve bundle stands out visually. STIR sequences can detect bone marrow changes near compressed areas. This combination gives radiologists a complete structural picture in one appointment.
For patients interested in proactive spinal health monitoring alongside other conditions, some imaging centers offer preventive scan packages that include the spine as part of a broader assessment.
Spinal Stenosis MRI vs Normal MRI
The clearest way to understand what stenosis looks like on MRI is to compare a normal spine against one with progressive narrowing.
In a normal spine MRI, the spinal canal appears as a rounded or oval structure with a visible ring of bright cerebrospinal fluid fully surrounding the nerve bundle. The individual nerve roots are visible as distinct structures within that fluid. Nothing is compressed or crowded.
As stenosis develops, that picture changes at each grade. The table below maps the progression, referenced against the Lee grading framework published in the Korean Journal of Radiology.
| Grade | Label | What the MRI Shows |
|---|---|---|
| Grade 0 | Normal | Full cerebrospinal fluid space surrounding the nerve bundle. Individual rootlets are clearly separated and visible. |
| Grade 1 | Mild | Some fluid remains visible. Rootlets are present but the space between them is noticeably reduced. |
| Grade 2 | Moderate | No fluid between individual rootlets, though each rootlet can still be distinguished from the others. |
| Grade 3 | Severe | No fluid and no separation between rootlets. The entire nerve bundle appears as a single compressed mass. |
These grades describe the imaging appearance. They are one input into clinical decisions, not a standalone treatment prescription. Many patients with Grade 2 findings have significant symptoms while others with Grade 3 findings remain functional with conservative management. The grade captures what the canal looks like; only a physician can assess what it means for you.
What Severe Spinal Stenosis Looks Like on MRI
Severe spinal stenosis (Grade 3) has a distinct appearance on MRI that radiologists and spine surgeons use to assess the degree of neural compression.
At Grade 3, the canal cross-sectional area at the most narrowed level may measure below 50 square millimeters. The cerebrospinal fluid space around the nerve bundle is completely gone. On T2-weighted images, the canal appears as a dark oval with no visible bright fluid surrounding the nerves. The nerve roots cannot be individually identified because they are compressed together.
Additional signs that radiologists associate with severe stenosis include:
- The sedimentation sign - in a normal resting scan, nerve roots settle toward the back of the dural sac. When stenosis is severe, the roots remain clumped together and cannot separate, even when the patient is lying down
- Spinal cord signal changes (myelopathy) - in cervical stenosis, bright areas within the cord on T2-weighted images indicate that cord tissue has been affected by sustained compression
- Dural sac obliteration - the sac surrounding the nerve bundle appears collapsed or flattened rather than round and fluid-filled
- Multilevel involvement - severe stenosis often occurs at more than one disc level simultaneously, and MRI can document all affected segments in a single exam
Imaging severity and symptom severity do not always match. Some patients with Grade 3 findings report manageable discomfort, while others with Grade 2 findings have significant limitations in daily activities. Radiologists document what the image shows. The clinical meaning is assessed by the treating physician in combination with your symptoms and functional history.
Lumbar vs Cervical Spinal Stenosis on MRI
Spinal stenosis can develop at any level of the spine, and MRI findings differ depending on whether the narrowing is in the lower back (lumbar) or the neck (cervical).
Lumbar spinal stenosis is the more common presentation, particularly in adults over 50. On MRI, lumbar stenosis typically shows disc bulging, facet joint enlargement, and ligamentum flavum thickening at one or more levels in the lower lumbar spine. The nerve bundle affected at this level is the cauda equina, a collection of roots rather than the spinal cord itself. The classic symptom pattern of leg cramping and pain that improves when sitting forward corresponds directly to the cauda equina compression visible on the scan.
Cervical spinal stenosis involves the spinal cord directly, and this distinction changes what radiologists look for on MRI. In the cervical spine, cord signal changes are possible where they are not in lumbar images. When cervical stenosis has been present long enough to affect cord tissue, MRI may show a bright signal within the cord on T2-weighted sequences, a finding called myelopathy. Patients with cervical stenosis who present with balance difficulty, arm weakness, or fine motor changes may also receive a brain MRI to rule out conditions that can produce similar neurological signs.
For a more detailed look at how MRI evaluates the neck in cervical stenosis, see our guide to cervical spine MRI.
MRI vs CT Scan for Spinal Stenosis

MRI is the preferred starting point, but CT scanning provides information that MRI cannot in specific situations, and understanding the difference helps you make sense of why your physician may order one or both.
CT imaging shows bone structure with precision. It measures exact bony canal dimensions, shows osteophytes (bone spurs) in sharp detail, and completes in 10 to 15 minutes versus 30 to 60 minutes for MRI. For patients with pacemakers or certain metal implants who cannot safely undergo MRI, CT is often the alternative.
CT myelography takes the bone detail of CT and adds contrast dye injected into the spinal fluid, producing highly detailed images of nerve root compression. Research has found that CT myelography can identify additional stenotic levels in multilevel cases that standard MRI may not fully capture. It requires a lumbar puncture to deliver the contrast, making it more invasive than either standard CT or MRI.
A side-by-side view of when each modality offers the most value:
- MRI is preferred when the primary concern is nerve compression, disc herniation, cord status, or soft tissue causes of stenosis
- CT is preferred when MRI is contraindicated due to implants, when precise bone measurements are needed for surgical planning, or when calcified disc fragments are suspected
- CT myelography is considered when MRI leaves questions unanswered, when multilevel disease makes it difficult to isolate the symptomatic level, or when MRI hardware artifacts interfere with image quality
Most spinal stenosis workups begin with MRI. CT is added when MRI does not fully answer the clinical question.
How MRI Results Can Guide Treatment Conversations

The purpose of a spinal stenosis MRI is not to issue a verdict but to give you and your physician a shared, objective picture of what is happening inside the canal. That picture then becomes one input alongside your symptoms, your functional limitations, and your goals for treatment.
Mild to moderate stenosis on MRI, where some cerebrospinal fluid space remains visible around the nerve roots and no cord signal changes are present, often corresponds to a treatment path that begins with conservative management. Physical therapy, anti-inflammatory medications, and activity adjustments address many cases at this severity level. Research has found that patients who begin physical therapy within six weeks of symptom onset may have lower rates of eventually needing surgical intervention.
Findings that may prompt a more urgent conversation with a spine specialist include:
- Grade 3 central stenosis with canal cross-sectional area below 50 square millimeters at the most compressed level
- Cervical cord signal changes indicating myelopathy from sustained cord compression
- Progressive neurological deficits such as worsening leg or arm weakness, or changes in bladder or bowel function
- Vertebral instability (spondylolisthesis) visible on MRI as a vertebral body that has shifted forward relative to the level below it
MRI results also help distinguish stenosis from conditions that produce similar symptoms but require different treatment. Tumors, infections, and vascular problems can all cause back pain and leg symptoms. Accurate imaging can prevent a misdiagnosis that leads to an ineffective treatment path.
For patients with existing spinal concerns alongside questions about bone health, a bone density test is sometimes recommended alongside spinal imaging, since osteoporosis can contribute to vertebral compression fractures that may co-exist with or appear similar to stenosis changes on initial evaluation.
What to Expect During a Spine MRI
A spine MRI takes 30 to 60 minutes. You will lie on a table that slides into the scanner, remain still throughout each imaging sequence, and hear loud tapping and buzzing sounds from the machine. Earplugs or headphones with music are standard at most facilities.
Preparation steps to keep in mind before your appointment:
- Remove all metal before entering - jewelry, hairpins, watches, hearing aids, and removable dental work must be removed before you enter the MRI room
- Disclose all implanted devices - pacemakers, cochlear implants, neurostimulators, and certain surgical hardware may affect MRI safety and require verification before scheduling
- Report kidney concerns - contrast-enhanced studies use a gadolinium injection and require kidney function verification for patients with kidney disease or diabetes
- Plan ahead for anxiety - patients who have concerns about claustrophobia during MRI can request anti-anxiety medication in advance; wide-bore scanners with a 70 cm opening accommodate the large majority of patients who find standard scanners uncomfortable
After the scan, a board-certified radiologist reviews the images and sends a written report to your ordering physician. Turnaround times vary by facility but are typically within 24 to 48 hours for non-emergency studies.
Frequently Asked Questions About Spinal Stenosis MRI
Does spinal stenosis show on MRI?
Yes. MRI is one of the most reliable ways to visualize spinal canal narrowing. The scan shows the canal dimensions, the structures narrowing it, and the nerves or spinal cord under pressure. Radiologists can identify the presence and grade of stenosis from a standard lumbar or cervical spine MRI, and the findings are documented in a written report that your physician uses for clinical decision-making.
Can an MRI tell how severe spinal stenosis is?
Yes. Radiologists use standardized grading systems, including the Lee grading scale, to classify stenosis from Grade 0 (normal) to Grade 3 (severe). The grade is determined by how much cerebrospinal fluid remains visible around the nerve bundle and whether individual nerve rootlets can still be distinguished. Canal cross-sectional area measurements add a second layer of objective data that complements the visual grade.
What does severe spinal stenosis look like on MRI?
Severe stenosis (Grade 3) appears as a canal where no cerebrospinal fluid space remains around the nerve bundle. The nerve roots appear compressed together as a single mass rather than as distinct structures. The dural sac may be flattened, and in cervical cases, the spinal cord itself may show bright signal changes on T2-weighted images, indicating the cord has been under sustained pressure long enough for tissue changes to occur.
What does spinal stenosis look like on MRI vs a normal spine?
A normal spine MRI shows clear cerebrospinal fluid surrounding the nerve bundle, with individual nerve roots visible as separate structures. In spinal stenosis, that fluid space is partially or fully gone. At mild and moderate grades, some fluid remains but the space between rootlets is reduced. At severe grades, no fluid is visible and the nerve roots appear crowded together as a single dense structure.
Is MRI or CT better for spinal stenosis?
MRI is generally the preferred first choice because it visualizes soft tissue, discs, ligaments, nerves, and the spinal cord with more clarity than CT. CT provides superior bone detail and completes more quickly. CT myelography, which adds contrast dye to a CT scan, can match or exceed MRI accuracy for complex or multilevel cases. Most clinicians begin with MRI and add CT if specific questions remain unanswered.
Can spinal stenosis MRI findings be worse than symptoms?
Yes. Research shows that a meaningful portion of adults over 50 have measurable canal narrowing visible on MRI without reporting significant symptoms. Stenosis is a structural finding, and whether it produces symptoms depends on factors beyond canal dimensions alone, including individual nerve tolerance, posture, activity habits, and the rate at which narrowing developed. MRI severity does not automatically predict symptom severity or the need for treatment.
When should spinal stenosis MRI results lead to treatment?
MRI findings are always considered alongside symptoms and functional impact. Mild to moderate stenosis without cord signal changes and with manageable symptoms often leads to a conservative treatment plan beginning with physical therapy. Findings that tend to prompt more active discussion include Grade 3 stenosis, cervical cord signal changes, progressive neurological deficits, and vertebral instability. Treatment decisions belong to the patient and their physician, with imaging providing the objective foundation for that conversation.
Can I get a spinal stenosis MRI without a referral?
In most clinical settings, an MRI for diagnosed or suspected spinal stenosis requires a physician's order to establish the appropriate clinical context. Craft Body Scan offers preventive imaging through its scan options that do not require a referral, providing a baseline picture of spinal and overall health that patients can share with their physician. Board-certified radiologists review every scan and provide a written report with plain-language findings.

Get Clearer Imaging Before Your Next Care Decision
If you want a clearer picture of your spinal health before your next doctor visit, Craft Body Scan's board-certified radiologists provide detailed imaging review and plain-language explanations of findings. No referral required. Results available to share with your physician or specialist. Want to know about preventive options beyond spine imaging? Ask about our whole-body MRI for a broader health picture in a single session.
Schedule a Scan