Medical Disclaimer: This article is intended for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making decisions about breast cancer screening.
If you have ever walked out of a doctor’s appointment with a referral for breast imaging and no real explanation of what comes next, you are not alone. The difference between a breast ultrasound and a mammogram trips up a lot of women — partly because both tests look at the same tissue, yet they work in completely different ways and catch completely different things. Knowing which one applies to you, and why, can change how you approach your own screening.
The short version: A mammogram uses low-dose X-ray to detect calcifications and structural changes across the entire breast, while a breast ultrasound uses sound waves to evaluate specific areas of tissue — particularly useful when dense tissue limits what a mammogram can see. Neither replaces the other. For many women, they work best together.
What Happens During a Mammogram
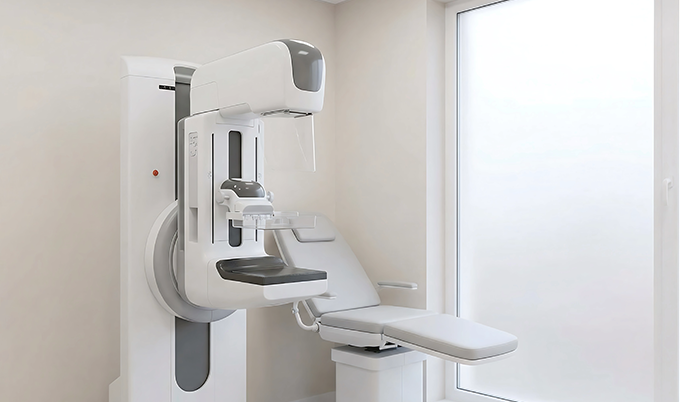
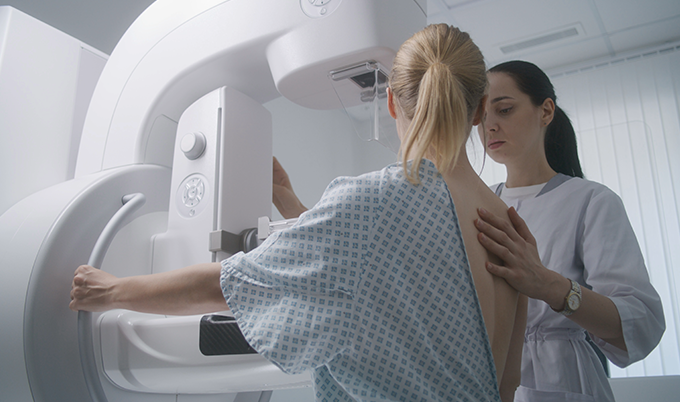
A mammogram is a low-dose X-ray of the breast. You stand at the machine, a technologist positions your breast between two compression plates, and the plates press the tissue flat for a few seconds while the image is captured. Most women find the compression uncomfortable rather than painful, though tenderness in the days before a period can make it feel sharper. The whole appointment typically takes less than 30 minutes.
The reason compression matters is physics. Flattening the tissue spreads it out, reduces the X-ray dose needed, and produces a clearer image. Two standard views are taken of each breast — one from above and one from an angle — giving radiologists a complete picture of the breast from different orientations.
What mammography is exceptionally good at detecting is microcalcifications. These are tiny calcium deposits, often invisible to any other imaging method, that can signal early ductal carcinoma in situ — cancer that has not yet left the milk ducts. That is a meaningful advantage. Mammography also maps the overall architecture of the breast across a wide field of view, which helps radiologists spot subtle distortions or asymmetries that warrant follow-up.
Where mammography runs into trouble is density. When breast tissue is dense — meaning it contains more glandular and connective tissue relative to fat — both the dense tissue and potential tumors appear white on the X-ray image. One conceals the other. Research published in PMC found mammographic sensitivity dropped to as low as 23.7% in women with heterogeneously dense breasts, compared to 82.2% in women with predominantly fatty tissue. That is not a minor difference. It is why roughly half of women who receive routine screening mammograms receive additional imaging afterward.
As of September 2024, the FDA now requires mammography providers nationwide to notify patients about their breast density in writing — a significant policy shift that gives women more information to act on.
What Happens During a Breast Ultrasound
A breast ultrasound is a very different experience. You lie on an exam table while a technologist or radiologist applies warm gel to the skin, then moves a handheld transducer across the breast. The transducer emits high-frequency sound waves that bounce off tissue and return as a real-time image on a screen. No radiation. No compression. No breath-holding. Most women find it entirely comfortable, and the exam typically takes 20 to 45 minutes depending on the area being evaluated.
Sound waves behave differently depending on what they hit. Fluid-filled cysts reflect sound one way, solid masses reflect it another. That distinction makes ultrasound particularly strong at characterizing a specific finding — determining whether a lump is a benign cyst full of fluid or a solid mass that warrants biopsy. It is also the preferred imaging method during pregnancy, since there is no ionizing radiation involved.
In dense breast tissue, where mammography loses sensitivity, ultrasound performs considerably better. A 2024 prospective study published in PMC found ultrasound sensitivity of 85.3% compared to mammography’s 61.8% in women with radiographically dense breasts. The ACRIN 6666 trial, one of the largest studies on supplemental screening, found that adding ultrasound to mammography in high-risk women with dense breasts detected an additional 3.7 cancers per 1,000 screens — cancers the mammogram alone had missed.
The tradeoff is specificity. Ultrasound finds more, but it also flags more findings that turn out to be benign. That leads to more follow-up appointments and occasional unnecessary biopsies, which is why supplemental ultrasound is typically recommended for women with a specific clinical reason rather than applied universally.
Mammogram vs Ultrasound: Side-by-Side Comparison
| Factor | Mammogram | Breast Ultrasound |
|---|---|---|
| Technology | Low-dose X-ray (ionizing radiation) | High-frequency sound waves (no radiation) |
| Best at detecting | Microcalcifications, tissue architecture changes, structural asymmetries | Cyst vs. solid mass distinction, cancers hidden by dense tissue |
| Dense tissue sensitivity | As low as 23.7% in heterogeneously dense tissue | 85.3% — significantly outperforms mammography in dense tissue |
| Exam experience | Compression required; mild discomfort; ~30 min | Gel + handheld wand; no compression; comfortable; 20–45 min |
| Safe in pregnancy? | Not preferred — radiation involved | Yes — preferred for pregnant patients |
| Recommended for | Average-risk women 40+, annual routine screening | Dense breasts, abnormal mammogram follow-up, under 30, symptoms |
Who Gets a Mammogram and Who Gets an Ultrasound
The two tests are not competing options on a menu. They serve different purposes and are recommended based on different clinical situations.
Mammography is the standard screening tool for women at average risk. The U.S. Preventive Services Task Force updated its guidelines in 2024 to recommend that women begin annual screening mammograms at age 40 — a shift from its previous guidance that had recommended starting at 50. The American Cancer Society continues to recommend annual mammograms starting at 40 for women at average risk, with the option to begin at 45.
Breast ultrasound is typically ordered in one of four scenarios:
- As a follow-up to an abnormal mammogram — If a mammogram shows a mass or area of concern, ultrasound helps characterize it further before a biopsy decision is made.
- For women under 30 or who are pregnant — In younger women where breast tissue is almost always dense, ultrasound is usually the first-line imaging tool. The absence of radiation also makes it appropriate during pregnancy.
- As supplemental screening for dense breasts — Women with heterogeneously dense or extremely dense breasts who have a normal mammogram may be offered supplemental ultrasound, particularly if they carry additional risk factors. The NCCN recommends supplemental MRI for women with extremely dense breasts, while the role of supplemental ultrasound is discussed in a shared decision-making context.
- For evaluating a specific symptom — A palpable lump, nipple discharge, or localized pain often prompts an ultrasound regardless of recent mammography status.
Screening vs Diagnostic: A Distinction That Matters
Both mammograms and ultrasounds can be either screening or diagnostic exams, and the difference affects how they are billed, how they are read, and what happens afterward.
A screening exam is performed on women with no current symptoms — the goal is to detect cancer before it announces itself. A diagnostic exam is performed when there is already a reason to look more carefully: a symptom, an abnormal screening result, or a prior history of breast cancer. Diagnostic exams are typically more thorough, may involve additional imaging views, and are often read in real time by a radiologist who may speak with you before you leave.
If your doctor orders a diagnostic mammogram rather than a screening mammogram, it does not mean something is necessarily wrong. It often simply means your clinical picture warrants a closer look from the start.
How Results Are Reported: The BI-RADS System
Both mammograms and ultrasounds use the same standardized reporting system developed by the American College of Radiology — called BI-RADS, which stands for Breast Imaging Reporting and Data System. The scale runs from 0 to 6.
| Score | Category | What it means | Next step |
|---|---|---|---|
| 0 | Incomplete | Additional imaging needed before a final assessment can be made — often an ultrasound or extra mammogram views. | Additional imaging |
| 1 | Negative | No significant finding. Breast tissue looks normal. | Routine screening |
| 2 | Benign finding | A definite benign finding is noted (e.g., cyst). Not cancer — documented for the record. | Routine screening |
| 3 | Probably benign | Almost certainly benign, but not definitively. Short-interval follow-up confirms stability. | 6-month follow-up |
| 4 | Suspicious | Not classic malignancy appearance, but suspicious enough to warrant tissue sampling. | Biopsy recommended |
| 5 | Highly suspicious | Very high probability of malignancy. All features strongly suggest cancer. | Biopsy required |
| 6 | Known malignancy | Biopsy-proven cancer already confirmed. Used when imaging evaluates treatment response. | Treatment planning |
A BI-RADS 0 on a mammogram is not a red flag — it most often means the radiologist wants an ultrasound or additional mammogram views before making a final assessment. Being called back after a screening mammogram is common and does not mean cancer has been found.
When Both Tests Work Together
For many women, the question is not mammogram or ultrasound — it is mammogram first, and then ultrasound if needed. That sequence reflects how breast cancer screening actually works in practice.
A mammogram covers the full breast and is excellent at detecting calcifications and tissue architecture changes across a large area. An ultrasound then steps in to characterize what the mammogram flagged, evaluate tissue that was difficult to see due to density, or provide supplemental coverage for women with higher risk profiles. Research consistently shows that combining the two modalities improves overall detection — the ACRIN 6666 data found that sensitivity for the combination of mammography plus ultrasound was 76%, versus each modality alone.
The emerging role of whole-body MRI is also worth noting for women with higher cancer risk. Craft Body Scan’s AI Whole-Body MRI uses advanced imaging to evaluate soft tissue throughout the body, which for high-risk women represents an additional layer of early detection beyond what any breast-specific imaging alone provides.
What to Ask Your Doctor Before Your Appointment
Going into a breast imaging appointment with a few questions prepared makes the process less passive and more useful.
Questions to Bring to Your Breast Imaging Appointment
- What is my breast density category, and what does it mean for my results?
- Is this a screening or diagnostic exam, and will that change how it is billed?
- If my mammogram shows dense tissue, will an ultrasound be offered the same day?
- How long will it take to receive results, and how will they be communicated?
- Based on my personal and family history, should I be discussing supplemental MRI?
Taking a Proactive Approach to Breast Health
The gap between screening mammography and early cancer detection is narrowing — but it requires patients to be active participants in that process. Knowing your breast density. Following up on callbacks without delay. Asking whether supplemental imaging applies to your situation. These decisions, made before anything is wrong, are what actually shift outcomes.
Preventive screening works precisely because it finds things that have not announced themselves yet. At Craft Body Scan, that philosophy drives everything we do — from our Full Body CT Scan to our AI Whole-Body MRI, reviewed by board-certified radiologists with detailed reports and follow-up on any findings. Transparent pricing. No referral required. Results you can actually understand.
Your health does not have to be reactive. Schedule your Craft Body Scan today and take the first step toward knowing what is happening inside your body before it becomes an emergency.