Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider regarding any medical condition or treatment plan.
Most people don’t see it coming.
They schedule a brain MRI after a headache that won’t quit, a balance issue they’ve been chalking up to getting older, or because someone finally talked them into a preventive scan. The report comes back. And somewhere in the clinical language, they find a phrase they’ve never heard before: chronic small vessel ischemic disease.
Nobody prepared them for that moment.
I’ve spent years working in preventive healthcare imaging, and what strikes me most about this condition is how consistently people encounter it this way — in a report, alone, without context. It’s one of the most common findings in adult brain imaging. Research puts the prevalence at roughly 5% of adults in their 50s and rising sharply from there — up to 80% of brain imaging in adults over 90 shows some degree of these changes. Common. And yet almost no one understands what those three words mean until they’re staring at them.
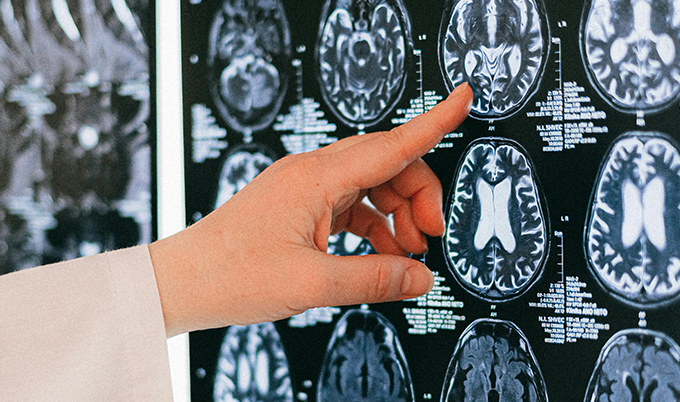
Here’s what chronic small vessel ischemic disease actually is: a condition in which the smallest blood vessels deep in the brain gradually become damaged or narrowed, restricting blood flow to the surrounding tissue over time. That restriction — called ischemia — leaves behind small areas of injury that show up on MRI as bright spots in the brain’s white matter. The changes build slowly. Quietly. Often without symptoms for years.
That’s the core answer. But what matters more than the definition is what you do with it — and that requires understanding what’s driving the damage, how serious it is in your specific case, and which interventions give you the best chance of stopping it from progressing further.
What Most People Get Wrong About This Diagnosis
The first thing I want to address is the fear. When people search for this diagnosis, a lot of what comes back makes it sound like a near-certain path to dementia or stroke. That’s not the full picture — and letting fear do the interpreting is one of the most costly mistakes you can make here.
Mild small vessel changes in a 65-year-old with well-controlled blood pressure? Those findings may remain stable for years. The condition exists on a spectrum, and where you fall on that spectrum depends heavily on what’s driving it and how aggressively those drivers get addressed.
This is not a passive condition that simply follows a predetermined course. It responds to treatment. People who bring blood pressure under consistent control and make the right lifestyle changes can dramatically slow its advancement — some essentially stop it.
There’s also a widespread belief that this is the same as having a stroke. It isn’t. A stroke is an acute event — a sudden blockage or bleed causing immediate, often dramatic neurological symptoms. Chronic small vessel ischemic disease is a slow, cumulative process. The damage builds over years, not hours. That distinction matters because the interventions look completely different.
This diagnosis is a data point. A warning with real clinical value. Not a verdict.

What Is Chronic Small Vessel Ischemic Disease — and What’s Actually Damaging Your Brain?
Aging is the baseline. Blood vessels get stiffer and more fragile with time — that’s biology. But aging alone rarely explains the full picture. Several conditions dramatically accelerate vessel damage in ways that go far beyond normal wear, and most of them are modifiable.
What Does It Look Like on an MRI?
On brain MRI, the condition shows up as white matter hyperintensities — bright spots in the brain’s deep connective tissue, called the white matter. Radiologists may describe them as periventricular changes (clustered near the fluid-filled ventricles), subcortical lesions (distributed deeper in white matter), or lacunar infarcts — pinhole-sized areas of dead tissue where a tiny vessel has fully blocked.
Severity matters. Mild findings in older adults are common and often require monitoring only. Moderate to severe changes — particularly in younger patients, or in anyone whose symptoms are worsening — warrant more active investigation and a real treatment response.
The Risk Factors That Drive It

Highest Impact
High Impact
High Impact
Moderate Impact
Moderate Impact
Variable
In most people, it’s a combination of several of these working together over decades. No single cause tells the whole story.
The Symptoms That Are Easy to Miss
What makes chronic small vessel ischemic disease particularly difficult to catch early is that it announces itself gently at first — if at all.
Memory lapses that seem like normal aging. A subtle slowing in how quickly you process information. A slight unsteadiness you attribute to inner ear issues. Mood changes — a flatness, an irritability — that feel more like life stress than anything medical. These are the early signals. And they’re easy to dismiss.
The clinical reality is uncomfortable: because these symptoms overlap so heavily with normal aging and depression, they get missed constantly. A patient who brings cognitive concerns to their primary care physician may leave with a mental health referral when what they actually needed was an MRI.
How Serious Is It — Really?
Here’s where I want to be direct rather than reassuring.
The severity depends on how much damage has accumulated, how quickly it’s progressing, and what underlying conditions are still active. Mild disease in someone who gets blood pressure under control and stays there? That’s a very different clinical situation than moderate-to-severe disease in someone with uncontrolled hypertension, active diabetes, and a 30-year smoking history.
What unchecked progression can lead to:
- Vascular dementia — the second most common form of dementia after Alzheimer’s, accounting for roughly 20% of all dementia cases worldwide. Small vessel disease is its leading cause. It develops as cumulative brain damage crosses a threshold that meaningfully impairs daily function — and unlike the cognitive changes that come before it, dementia is not reversible.
- Ischemic stroke — specifically lacunar strokes, caused by complete blockage of already-damaged tiny vessels. These may not cause obvious immediate symptoms, but they add to the cumulative injury burden and raise the risk of subsequent stroke events significantly.
- Progressive mobility loss — as motor pathways through the white matter become increasingly disrupted, walking difficulties worsen in ways that affect independence. Driving. Stairs. Moving through a room without holding something.
- Accelerated cognitive decline — people with more extensive white matter changes show faster progression toward dementia than those with minimal findings, independent of other factors.
That’s the trajectory without meaningful intervention. Which is exactly why finding this early — before the functional threshold is crossed — changes what’s possible.
How Small Vessel Disease Is Diagnosed
There’s no blood test for this. No physical exam finding that reliably catches it early. Imaging is the only way in — which is part of why it goes undetected for so long in people who never pursue proactive brain screening.
A full diagnostic workup typically includes:
| Diagnostic Tool | What It Shows | Clinical Role | Key Limitation |
|---|---|---|---|
| Brain MRI (FLAIR/T2) | White matter hyperintensities, lacunar infarcts, lesion distribution | Gold standard — detects changes before symptoms | Higher cost; limited access in some areas |
| CT Brain Scan | Structural changes, calcified lesions, large infarcts | Rules out structural causes; useful if MRI unavailable | Less sensitive for early or subtle white matter changes |
| Neuropsychological Testing | Memory, attention, processing speed, executive function | Quantifies functional impact of imaging findings | Does not show anatomical location of damage |
| Vascular Risk Workup | BP trends, HbA1c, lipid panel, ECG (atrial fibrillation) | Identifies modifiable drivers; guides treatment targets | Does not visualize brain tissue directly |
At Craft Body Scan, our brain MRI scan is designed for proactive screening — not waiting rooms and referral queues. It gives you and your physician the imaging data needed to make informed decisions about your brain health, without requiring a symptom crisis as the entry point.

Managing Chronic Small Vessel Ischemic Disease — What Actually Works
The lesions don’t heal. Accept that up front — it makes the rest of this more useful.
What you can change is how fast the condition moves. And the pace of small vessel disease is more responsive to treatment than most people realize.
Getting and keeping BP below 130/80 mmHg is the single most impactful intervention available. Every point of sustained systolic reduction meaningfully slows new white matter lesion development. This requires consistency — not just before appointments.
For type 2 diabetes, HbA1c consistently below 7% measurably slows the pace of microvascular injury throughout the body. Brain vessels benefit alongside kidneys and eyes. Inconsistent control keeps the damage accumulating.
Beyond cholesterol reduction, statins carry anti-inflammatory properties at the vascular level. Increasingly recommended for confirmed small vessel disease even at moderate cholesterol levels because of their direct effect on vessel wall inflammation.
Low-dose aspirin or similar agents may be appropriate depending on individual stroke risk profile. Discuss with a neurologist or cardiologist rather than self-prescribing — not appropriate for all patients.
Targeted physical therapy maintains gait mechanics and balance. Cognitive rehabilitation and structured brain training support executive function through compensatory strategies as the disease progresses.
Typically every one to two years — to confirm whether management is actually working or whether the approach needs adjustment. Imaging tracks lesion burden; testing tracks functional impact.
The Daily Habits That Change the Trajectory
Medical treatment works best when daily habits aren’t working against it. Here’s what has the strongest evidence behind it — not general wellness advice, but interventions with documented effects on cerebrovascular health specifically.
Questions to Ask Your Doctor After a Small Vessel Disease Finding
- What is the severity grade of my white matter changes — mild, moderate, or severe?
- Which of my current risk factors are most likely driving this finding?
- What blood pressure target should I be hitting, and how do we get there?
- Should I have neuropsychological testing to quantify functional impact?
- Am I a candidate for statin or antiplatelet therapy?
- Have I been evaluated for sleep apnea?
- How frequently should I repeat brain MRI imaging to monitor progression?

What Early Detection Actually Changes
The people who do best with this diagnosis are the ones who found out early. Not after a stroke. Not after dementia has taken functional hold. Before the threshold where meaningful, irreversible change has accumulated.
That window — where imaging shows what’s happening and treatment has real leverage — is the window most people miss. Because they’re waiting for symptoms. Because imaging requires a referral and a reason. Because the system is built for reaction, not prevention.
Our brain MRI gives you and your physician the imaging data needed to make targeted, informed treatment decisions — no symptom required as an entry point.
Our brain MRI scan at Craft Body Scan gives you a clear picture of your brain’s structural health today — not after a crisis forces the question. For a broader look at the cardiovascular risk factors that drive small vessel disease, our full body scan gives you and your physician the complete data set needed to make targeted, informed treatment decisions.
Chronic small vessel ischemic disease doesn’t have to define what comes next. But ignoring it does. Good information. Early. That’s what changes the outcome.
Schedule your scan today and take that first step.
Schedule your Craft Body Scan today
Frequently Asked Questions About Chronic Small Vessel Ischemic Disease
Is chronic small vessel ischemic disease the same as a stroke?
No. A stroke is an acute event – sudden blockage or rupture causing immediate neurological symptoms. Chronic small vessel ischemic disease is a slow, cumulative process with damage building over years. The two are related in that severe small vessel disease raises stroke risk, and people with the condition can experience small lacunar strokes caused by complete blockage of an already-damaged tiny vessel. But they’re distinct conditions requiring different approaches.
Can white matter lesions heal or disappear?
Once formed, white matter lesions are permanent. Current treatments don’t reverse existing tissue damage. What does respond to treatment is the rate of new lesion formation – aggressive blood pressure and metabolic control can substantially slow or pause the progression of new changes, which is why finding this early matters so much.
What do "mild," "moderate," and "severe" mean on an MRI report?
These terms describe the volume and distribution of white matter changes visible on imaging. Mild findings are common in adults over 60 and often require monitoring only. Moderate disease warrants active risk factor management and regular follow-up. Severe disease is associated with meaningful cognitive and functional impairment and elevated dementia and stroke risk. The grade isn’t a fixed fate – it’s a baseline to act from.
How quickly does this condition progress?
Progression varies significantly between individuals. With well-controlled risk factors, lesions may remain stable for years. With uncontrolled hypertension or diabetes, substantial progression can occur within 12 to 24 months. This variability is exactly why follow-up imaging matters – it tells you directly whether your current management approach is working or whether it needs adjustment.
Should I get a brain MRI if I have risk factors but no symptoms?
If you have multiple risk factors – particularly hypertension, type 2 diabetes, a history of smoking, or a family history of vascular dementia or early stroke – proactive brain imaging is worth a real conversation with your physician. Detecting changes before symptoms appear gives you the most options and the most time to act.
Does chronic small vessel ischemic disease always lead to dementia?
No. Many people with mild to moderate small vessel disease never develop dementia, particularly when risk factors are well managed over time. The risk rises with disease severity, additional stroke events, and sustained poor control of blood pressure and blood sugar. Prognosis here is not fixed – it’s directly shaped by what you do with the diagnosis.
How is this different from Alzheimer's disease?
Alzheimer’s disease involves accumulation of amyloid plaques and tau tangles in brain tissue. Small vessel disease causes vascular dementia through restricted blood flow and cumulative tissue injury. They produce different patterns on imaging – Alzheimer’s typically shows cortical atrophy and hippocampal changes; small vessel disease shows white matter changes in deeper brain structures. The two conditions frequently coexist in older adults, which is why imaging that can characterize both patterns matters for accurate diagnosis and appropriate treatment planning.