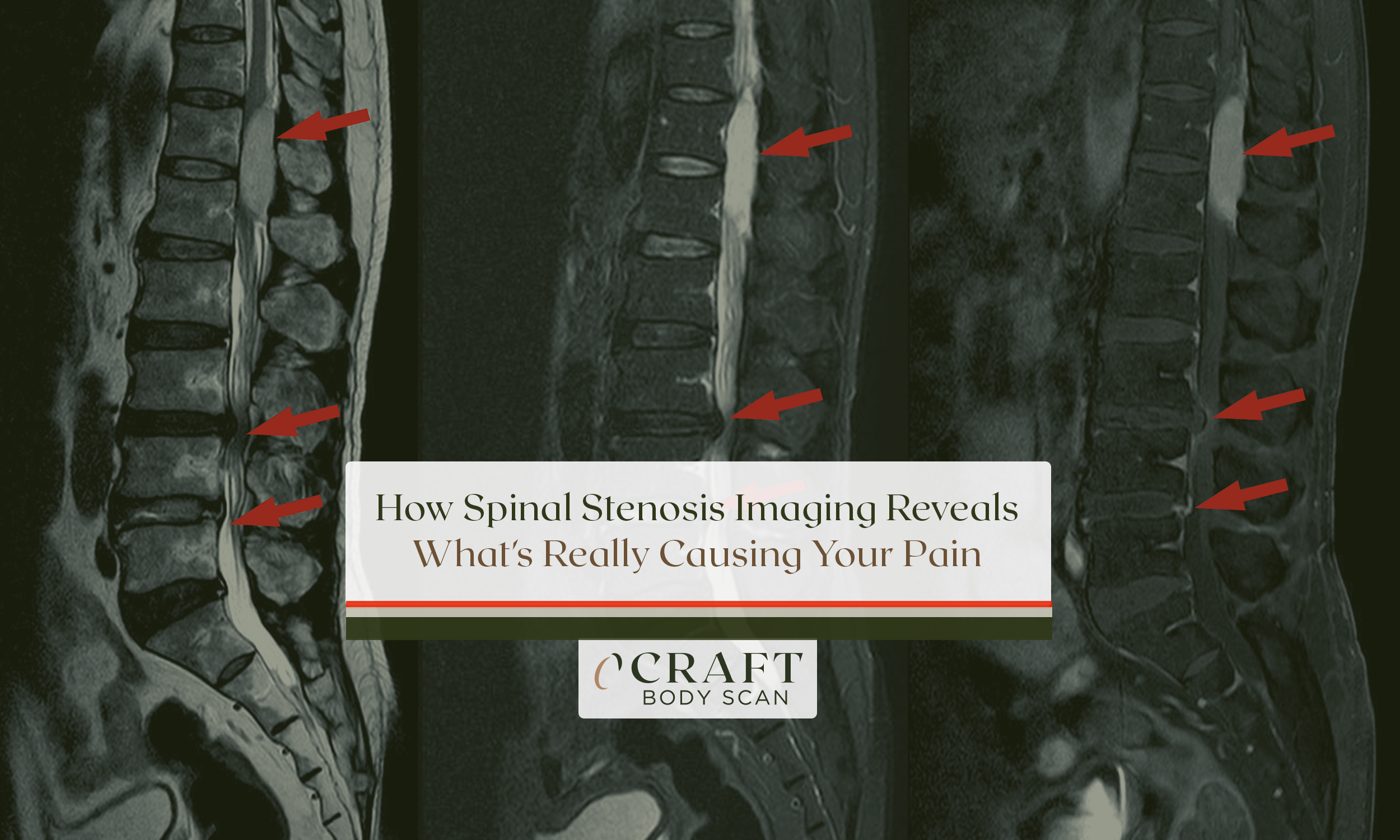
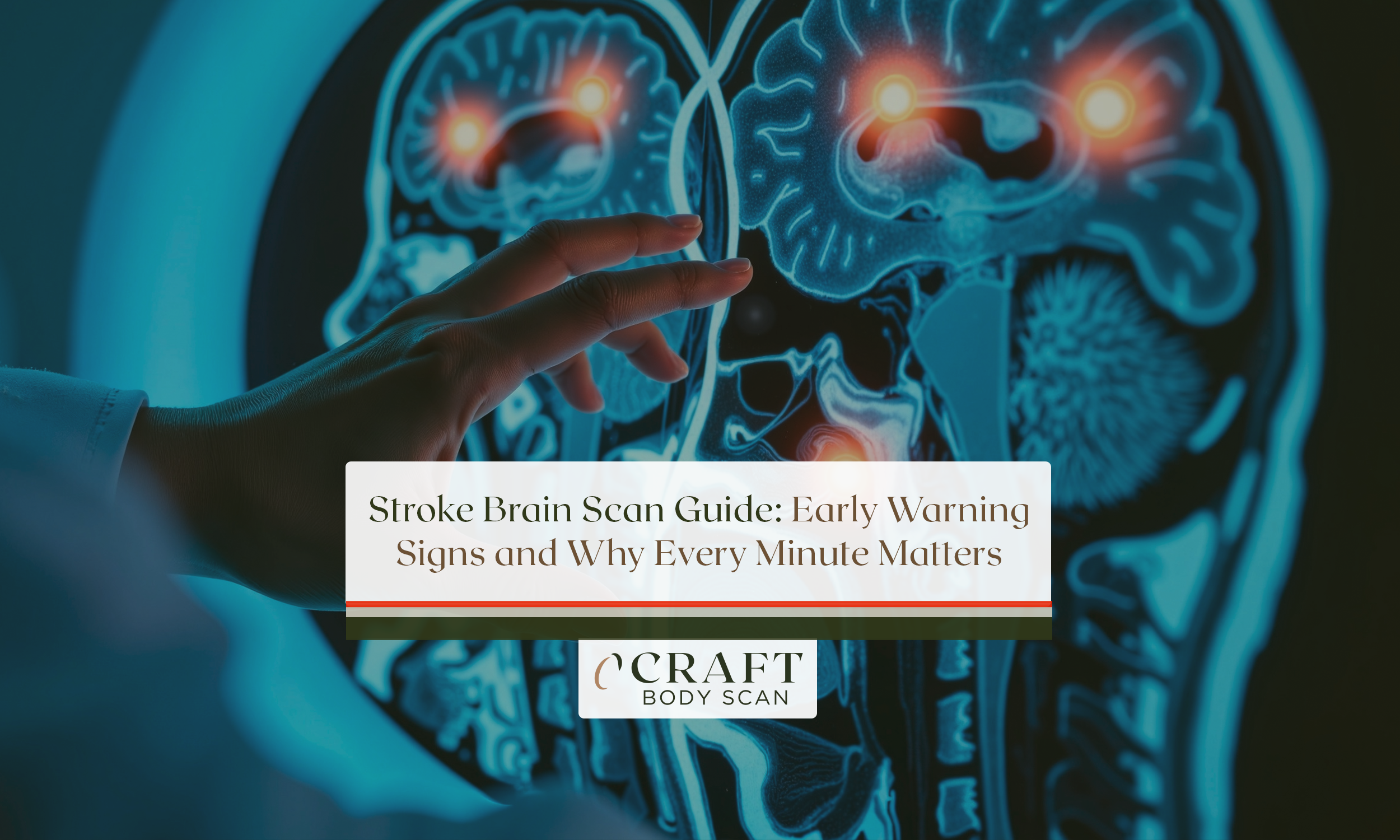
When your doctor orders a cervical spine MRI, you’re probably wondering why you need this test. As someone who specializes in preventive imaging, I’ve helped thousands of patients understand how this painless scan provides answers simpler tests can’t deliver.
A cervical spine MRI uses magnetic fields and radio waves to create detailed 3D images of your neck’s soft tissues. These images reveal your spinal discs, spinal cord, nerves, and surrounding structures. Unlike X-rays that only show bones, cervical spine MRI imaging reveals herniated discs, spinal stenosis, tumors, and infections affecting the seven vertebrae in your neck. The scan typically takes 20-45 minutes. It requires no radiation exposure.
Why Doctors Order Cervical Spine MRI Scans for Neck Pain

Your doctor orders a cervical spine MRI when symptoms suggest something more than simple muscle strain.
The most common trigger is persistent neck pain that hasn’t improved after 6 weeks of conservative treatment. This includes physical therapy, rest, and medication.
Pain radiating down your arms changes everything. When neck pain travels into your shoulders, arms, or hands – especially with numbness or tingling – your doctor suspects nerve root compression. This radiculopathy occurs when herniated discs or bone spurs press against nerves exiting your spinal column. A cervical spine MRI pinpoints exactly which nerve is compressed and why.
Motor symptoms escalate urgency. If you’re experiencing weakness in your hands, difficulty with fine motor tasks like buttoning shirts, or problems walking, these signal potential spinal cord compression.
Doctors order emergency cervical spine MRI scans when patients report bladder control issues or progressive weakness. These symptoms indicate cervical myelopathy requiring immediate intervention.
 Common Reasons Doctors Order Cervical Spine MRI
Common Reasons Doctors Order Cervical Spine MRI
- Persistent neck pain lasting more than 6 weeks without improvement
- Radiating arm pain with numbness or tingling (radiculopathy)
- Motor weakness affecting hands, arms, or legs
- Post-trauma assessment after car accidents or significant falls
- Pre-surgical planning for cervical fusion or disc replacement
- Suspected tumors or infections with unexplained symptoms
- Multiple sclerosis evaluation or disease monitoring
Post-Trauma Cervical Spine MRI Evaluation
Post-trauma evaluation protects against hidden injuries. After car accidents or significant falls, doctors use cervical spine MRI to assess soft tissue damage that won’t show on X-rays.
Whiplash injuries can cause disc herniation, ligament tears, or subtle spinal cord contusions. These are visible only through magnetic resonance imaging.
Cervical Spine MRI for Surgical Planning
Pre-surgical planning demands precise visualization. Before performing cervical fusion, laminectomy, or disc replacement surgery, surgeons need detailed maps of your anatomy.
Cervical spine MRI scans reveal disc degeneration severity, spinal canal narrowing extent, and nerve compression locations. This information determines surgical approach and expected outcomes.
Suspected tumors or infections require definitive diagnosis. When patients present with unexplained neck pain accompanied by fever, weight loss, or night sweats, doctors order cervical spine MRI with contrast. The scan detects spinal tumors or infections like osteomyelitis. It distinguishes between benign and malignant growths affecting vertebrae or spinal cord.
Multiple Sclerosis and Cervical Spine MRI
Multiple sclerosis evaluation needs cervical spine MRI imaging. Neurologists order this scan alongside brain MRI when diagnosing or monitoring MS patients.
Demyelinating lesions in the spinal cord appear as bright spots on T2-weighted images. This helps confirm diagnosis and track disease progression.
Follow-up imaging monitors treatment effectiveness. Patients who’ve undergone previous spine surgery receive interval cervical spine MRI scans. These assess healing, detect recurrent disc herniation, or identify complications like post-surgical infection or hardware failure.
What Conditions Cervical Spine MRI Detects in Your Neck
Herniated discs appear as bulging material protruding beyond normal disc boundaries on cervical spine MRI images. The C6-C7 level (between the sixth and seventh cervical vertebrae) experiences the highest herniation rates. C5-C6 follows closely behind.
Research shows 98% of patients with lumbar disc herniation also demonstrate cervical disc degeneration on cervical spine MRI. This suggests degenerative disc disease affects the entire spine systemically.
| Condition Detected | How It Appears on Cervical Spine MRI | Clinical Significance |
|---|---|---|
| Herniated Disc | Bulging material beyond disc boundaries | Nerve compression, arm pain |
| Spinal Stenosis | Narrowed spinal canal, compressed cord | Myelopathy, walking difficulties |
| Degenerative Disc Disease | Dark signal intensity, decreased disc height | Chronic neck pain, stiffness |
| Tumors | Abnormal masses with contrast enhancement | Requires biopsy, treatment planning |
| Infections | Inflammation, fluid collections | Emergency treatment needed |
Spinal Stenosis Detection on Cervical Spine MRI
Spinal stenosis narrows the canal housing your spinal cord. This condition affects approximately 1 in 1,000 people over 65. It affects 5 in 1,000 over age 50 in North America.
Cervical spine MRI reveals whether stenosis results from herniated discs, thickened ligaments, bone spurs, or combinations of these factors. Radiologists grade stenosis severity using standardized systems. These measure cerebrospinal fluid space obliteration and spinal cord deformity.
Nerve Root Compression Patterns
Nerve root compression shows precisely which nerves are pinched on cervical spine MRI images. Each cervical nerve controls specific muscle groups and sensation areas.
C5 nerve compression causes shoulder weakness and deltoid numbness. C6 compression affects biceps strength and thumb sensation. C7 compression weakens triceps and causes middle finger numbness. C8 compression impacts hand grip and pinky finger sensation.
Degenerative Disc Disease on Cervical Spine MRI
Degenerative disc disease appears as signal intensity changes. Healthy discs appear bright on T2-weighted cervical spine MRI images due to high water content.
Degenerated discs show decreased signal intensity – appearing darker – as they lose hydration. Advanced degeneration includes disc height loss, bone marrow changes in adjacent vertebrae (Modic changes), and osteophyte (bone spur) formation.
Spinal cord signal abnormalities indicate serious pathology. Bright signal changes within the cord on T2-weighted images suggest myelomalacia. This is spinal cord softening from chronic compression, acute injury, inflammation, or tumors. These findings often correlate with clinical myelopathy symptoms and predict surgical outcomes.
Tumor Detection with Cervical Spine MRI
Tumors appear as abnormal masses with characteristic patterns. Intradural extramedullary tumors (meningiomas, nerve sheath tumors) grow inside the spinal canal but outside the cord. Intramedullary tumors (astrocytomas, ependymomas) arise within the spinal cord itself.
Metastatic tumors often affect vertebral bodies. Contrast-enhanced cervical spine MRI helps distinguish tumor types and guides biopsy planning.
Infections show inflammation and fluid collections on cervical spine MRI images. Discitis (disc infection) appears as disc signal changes with adjacent vertebral inflammation. Epidural abscesses appear as fluid collections compressing the spinal cord. These are surgical emergencies requiring immediate drainage.
Osteomyelitis shows bone marrow signal abnormalities indicating vertebral infection.
Congenital Abnormalities Revealed by Cervical Spine MRI
Congenital abnormalities reveal developmental variations. Cervical spine MRI identifies conditions present since birth. These include os odontoideum (abnormal C1-C2 articulation), Klippel-Feil syndrome (fused cervical vertebrae), Chiari malformations (cerebellar tissue extending into spinal canal), and syringomyelia (fluid-filled cavities within the spinal cord).
Ligamentous injuries appear as signal abnormalities or discontinuity. Posterior longitudinal ligament ossification (OPLL) – more common in Asian populations – appears as calcified tissue compressing the spinal cord. Ligament tears from trauma show increased signal intensity on certain cervical spine MRI sequences.
Vascular malformations carry bleeding risk. Arteriovenous malformations and spinal aneurysms appear as abnormal blood vessel clusters. These rare conditions can cause sudden neurological deterioration if they rupture. Cervical spine MRI with angiography sequences helps identify these vascular abnormalities.
Understanding How Cervical Spine MRI Technology Works
The physics behind cervical spine MRI exploits hydrogen atoms in your body’s water molecules. When you enter the powerful magnetic field (typically 1.5 or 3 Tesla), hydrogen protons align with that field. They align like compass needles pointing north.
Radiofrequency pulses then knock these protons out of alignment.
As protons realign, they emit radio signals your body creates. The MRI scanner’s sensors detect these signals. Computers convert them into cross-sectional images – called “slices” – showing tissue differences.
Each slice reveals anatomical structures at a specific level. This is much like bread slices show the loaf’s interior. A complete cervical spine MRI produces hundreds of these slices from multiple angles.
Different tissue types emit distinct signals. Cerebrospinal fluid appears bright on T2-weighted images. Discs show varying signal intensity based on hydration. Bone appears dark due to low hydrogen content.
Spinal cord displays intermediate signal intensity. Fat produces high signal on T1-weighted images. These signal differences allow radiologists to distinguish normal from abnormal tissues.
Multiple Imaging Sequences in Cervical Spine MRI
Multiple imaging sequences capture different information. T1-weighted images excel at showing anatomy. T2-weighted images highlight fluid and pathology.
STIR (Short Tau Inversion Recovery) sequences suppress fat signal to reveal bone marrow edema. Gradient echo sequences detect blood products. Each sequence takes 3-5 minutes to complete.
Contrast agents sometimes enhance cervical spine MRI visualization. Gadolinium-based contrast injected through an IV accumulates in areas with abnormal blood flow. This includes tumors, infections, and inflamed tissues.
Post-contrast images show enhancement patterns helping distinguish between different pathology types. Patients with kidney disease require kidney function testing before receiving contrast.
Imaging Planes and Specialized Coils
The imaging plane determines the view. Sagittal images slice through your neck from right to left. They show all vertebrae in profile – ideal for assessing disc height and spinal alignment.
Axial images cut horizontally across your neck. They show spinal cord cross-sections and nerve root exits – perfect for evaluating stenosis and disc herniations. Coronal images provide front-to-back views. These are useful for detecting scoliosis or lateral abnormalities.
Specialized coils focus magnetic fields. Technicians place a neck coil – a curved frame – around your cervical spine before scanning. This dedicated hardware optimizes image quality for your specific anatomy. It produces clearer pictures than body coils designed for larger areas.
What to Expect During Your Cervical Spine MRI Appointment
The preparation phase starts when you change into a hospital gown. Remove all metal objects – jewelry, watches, hairpins, eyeglasses, hearing aids, removable dental work.
Metal interferes with magnetic fields or becomes dangerous projectiles in the scanner’s powerful magnet.
Inform staff about any implanted medical devices. Pacemakers, cochlear implants, neurostimulators, and some orthopedic hardware may contraindicate cervical spine MRI. Modern devices increasingly use MRI-compatible materials. However, technicians need device information (manufacturer, model number) to verify safety.
Previous surgical clips, plates, or screws usually pose no problems but require documentation.
Your medical history determines contrast use. If your doctor ordered contrast-enhanced cervical spine MRI, staff will insert an IV line before scanning. Diabetic patients or those with kidney disease may need recent creatinine lab results. These confirm adequate kidney function.
Allergies to gadolinium contrast are rare but possible. Report any previous contrast reactions.
 Cervical Spine MRI Safety Checklist
Cervical Spine MRI Safety Checklist
- Remove all metal objects before entering the scanning room
- Inform technicians about implanted devices (pacemakers, cochlear implants)
- Report kidney problems if contrast will be used
- Mention claustrophobia concerns to receive anxiety medication if needed
- Bring headphones or earplugs for the loud scanning noises
- Plan for 20-45 minutes of remaining completely still
- Arrange transportation if receiving sedation medication
Positioning and Scanning Process
Positioning matters for cervical spine MRI image quality. You’ll lie face-up on a narrow motorized table. Your head goes in a padded holder. Technicians position the neck coil around your cervical spine.
They may place padding under your knees for comfort. They provide a call button in your hand. The table then slides into the scanner’s tunnel opening.
The scanning process requires absolute stillness. Any movement – even swallowing or shifting position – blurs cervical spine MRI images. This necessitates sequence repeats, extending your scan time.
The machine makes loud thumping, banging, and buzzing noises. These occur as magnetic gradients switch on and off. Most facilities provide earplugs or headphones playing music.
The environment feels enclosed but manageable. Your head enters the tunnel opening while your body remains partially outside. Modern scanners feature wider bores (openings) than older machines.
Open MRI scanners – with wider openings on the sides – accommodate claustrophobic patients. They may produce slightly lower image quality.
The duration ranges from 20 to 45 minutes for standard cervical spine MRI. Contrast-enhanced studies take longer – up to 60 minutes total. Each sequence requires 3-5 minutes.
Technicians monitoring from an adjacent control room can communicate through speakers. They see you via camera throughout the scan.
Post-Procedure Recovery
Post-procedure recovery is immediate. Once scanning completes, the table slides out. Technicians remove the coil. You can immediately resume normal activities unless you received anxiety medication before the scan.
If contrast was used, drink extra fluids to help flush it from your system. Kidneys eliminate gadolinium naturally within 24 hours.
Understanding Your Cervical Spine MRI Results and Next Steps
A board-certified radiologist analyzes your cervical spine MRI images, typically within 24-48 hours. They examine hundreds of slices looking for disc abnormalities, stenosis, cord compression, nerve impingement, signal changes, and any unexpected findings.
The radiologist documents observations in a detailed report sent to your ordering physician.
Your doctor interprets results in clinical context. Cervical spine MRI findings correlate with your symptoms, physical examination, and medical history. Asymptomatic disc bulges are common. Research shows 22.7% of symptom-free volunteers demonstrate spinal stenosis on imaging.
Not every abnormality requires treatment.
Mild findings often warrant conservative management. Small disc bulges without nerve compression typically improve with physical therapy. Anti-inflammatory medications and activity modification help.
Your doctor monitors symptoms rather than rushing to intervention.
Moderate to severe findings may require specialist referral. Significant spinal cord compression, large disc herniations causing progressive weakness, or tumors necessitate neurosurgeon or orthopedic spine surgeon evaluation. These specialists use cervical spine MRI images alongside your symptoms. They develop treatment plans based on complete clinical information.
Surgical decisions depend on multiple factors. MRI severity, symptom duration, conservative treatment failure, neurological deficits, and patient preferences all influence whether surgery becomes necessary. Imaging guides surgical approach – anterior (front of neck) versus posterior (back of neck). It helps surgeons plan decompression extent.
Cervical Spine MRI Cost and Access Considerations
Cervical spine MRI costs range from $400 to $7,000 without insurance. This depends on facility type and geographic location. Hospital-based imaging centers typically charge more than independent outpatient facilities.
With insurance, out-of-pocket costs range from $50 to $500. This depends on deductibles and co-insurance.
Prior authorization requirements vary by insurance. Many insurers require documentation of conservative treatment failure. They require this before approving cervical spine MRI for non-urgent indications.
Emergency presentations receive immediate approval. These include trauma, progressive neurological deficits, and suspected cord compression.
Scheduling timeframes depend on urgency. Emergent scans happen within hours. Urgent scans (progressive symptoms) occur within days. Routine scans may require waiting weeks at busy facilities.
Independent imaging centers often offer shorter wait times than hospital departments.
Advanced Cervical Spine MRI Techniques
Weight-bearing MRI technology reveals dynamic compression. Traditional cervical spine MRI scans patients lying flat – gravity doesn’t compress discs. Newer systems tilt patients upright or image them sitting.
This reveals disc herniations and stenosis visible only under body weight. Flexion-extension views show instability by imaging the neck in different positions.
High-resolution 3 Tesla scanners provide superior detail. Stronger magnetic fields produce clearer cervical spine MRI images. This is particularly important for small structures like nerve roots. Some facilities offer 3T scanning as a premium option. Others use it routinely for complex cases.
Diffusion tensor imaging tracks nerve fiber integrity. This advanced cervical spine MRI technique maps white matter tracts within the spinal cord. It helps predict surgical outcomes in myelopathy patients. It distinguishes reversible from irreversible cord damage.
Making Informed Decisions About Cervical Spine MRI Imaging

Understanding when cervical spine MRI adds value helps you advocate for appropriate care. Acute neck pain lasting less than 6 weeks rarely requires imaging. Exceptions exist when red flags are present.
These include trauma, fever, progressive weakness, or bowel/bladder changes. Conservative treatment resolves most simple neck strains.
Persistent or radiating symptoms justify cervical spine MRI. When neck pain extends beyond 6 weeks despite appropriate treatment, imaging provides clarity. When symptoms radiate into arms with numbness or weakness, cervical spine MRI provides diagnostic information. This guides treatment adjustments.
At Craft Body Scan, we understand the anxiety accompanying neck symptoms. Our board-certified radiologists provide detailed interpretations. These help you and your physician make informed treatment decisions.
While we focus on preventive full body scanning, we recognize the importance of targeted diagnostic imaging. We understand when symptoms warrant evaluation.
The cervical spine MRI remains the gold standard for visualizing soft tissue pathology in your neck. This non-invasive, radiation-free test provides information unavailable through other imaging modalities. This information can prevent permanent neurological damage through timely intervention. According to the American College of Radiology, MRI is the preferred imaging modality for evaluating cervical spine pathology when neurological symptoms are present.
Whether your doctor ordered cervical spine MRI for persistent pain, radiating symptoms, or pre-surgical planning, understanding the test’s capabilities helps reduce anxiety. It prepares you for the examination.
The 20-45 minutes you spend in the scanner may provide answers that finally explain your symptoms. These answers guide you toward effective treatment. Schedule your consultation to discuss whether cervical spine imaging is right for your situation.
Cervical Spine MRI FAQs
A standard cervical spine MRI takes 20-45 minutes to complete. Each imaging sequence (T1-weighted, T2-weighted, STIR) requires 3-5 minutes of scanning time. If your doctor orders contrast enhancement with gadolinium injection, the total exam time extends to approximately 60 minutes. The actual time can vary based on the number of sequences needed, whether you need to repeat any sequences due to movement, and the specific protocols your imaging facility uses. You must remain completely still throughout the entire scan to ensure clear images.
Most patients tolerate cervical spine MRI well because your head enters the tunnel while much of your body remains outside the scanner opening. Modern MRI machines have wider bores (openings) that feel less confining than older models. If you have significant claustrophobia, inform your doctor beforehand—they can prescribe anti-anxiety medication to take before the scan. Some facilities offer open MRI scanners with openings on the sides, though these may produce slightly lower image quality. Breathing exercises, closing your eyes before entering the scanner, and listening to music through headphones can also help manage anxiety.
Yes, cervical spine MRI is excellent at showing pinched nerves (nerve root compression). The scan reveals what’s compressing each nerve—whether it’s a herniated disc, bone spur, thickened ligament, or spinal stenosis. MRI shows both the compressed nerve itself and the surrounding soft tissues causing the compression with millimeter precision. Each cervical nerve controls specific areas: C5 affects shoulder strength, C6 affects biceps and thumb sensation, C7 affects triceps and middle finger, and C8 affects hand grip and pinky finger. Your radiologist can identify exactly which nerve root is compressed and correlate this with your symptoms.
X-rays only show bones and cannot visualize soft tissues like discs, nerves, ligaments, or the spinal cord itself. Many serious cervical spine conditions—including herniated discs, spinal cord compression, tumors, infections, and nerve root impingement—are completely invisible on X-rays but show clearly on MRI. While X-rays can detect fractures, alignment problems, and advanced arthritis, they miss the soft tissue pathology that causes most neck pain and arm symptoms. MRI uses magnetic fields and radio waves (no radiation) to create detailed images of all tissues in your neck, making it the gold standard for evaluating persistent neck pain, radiating arm symptoms, or suspected spinal cord problems.
It depends on the specific device and when it was implanted. Many modern pacemakers, artificial joints, surgical plates, and screws are now made from MRI-compatible materials that allow safe scanning. However, older pacemakers, cochlear implants, certain aneurysm clips, and some neurostimulators may absolutely contraindicate MRI. You must inform the imaging facility about ALL implanted devices before scheduling, including the manufacturer and model number if possible. The facility will verify safety with the device manufacturer. If you cannot safely undergo MRI, your doctor may order alternative imaging such as CT myelography to evaluate your cervical spine.
This is extremely common and doesn’t necessarily mean you need treatment. Research shows that 22.7% of people with no neck pain or arm symptoms have spinal stenosis visible on MRI, and disc bulges are even more common in asymptomatic individuals. Many degenerative changes are simply part of normal aging and don’t cause problems. Your doctor interprets MRI findings in the context of your symptoms, physical examination, and medical history. Abnormalities that don’t correlate with your symptoms typically don’t require intervention. Treatment decisions are based on how you feel clinically and whether imaging findings explain your specific symptoms, not solely on what the MRI shows.