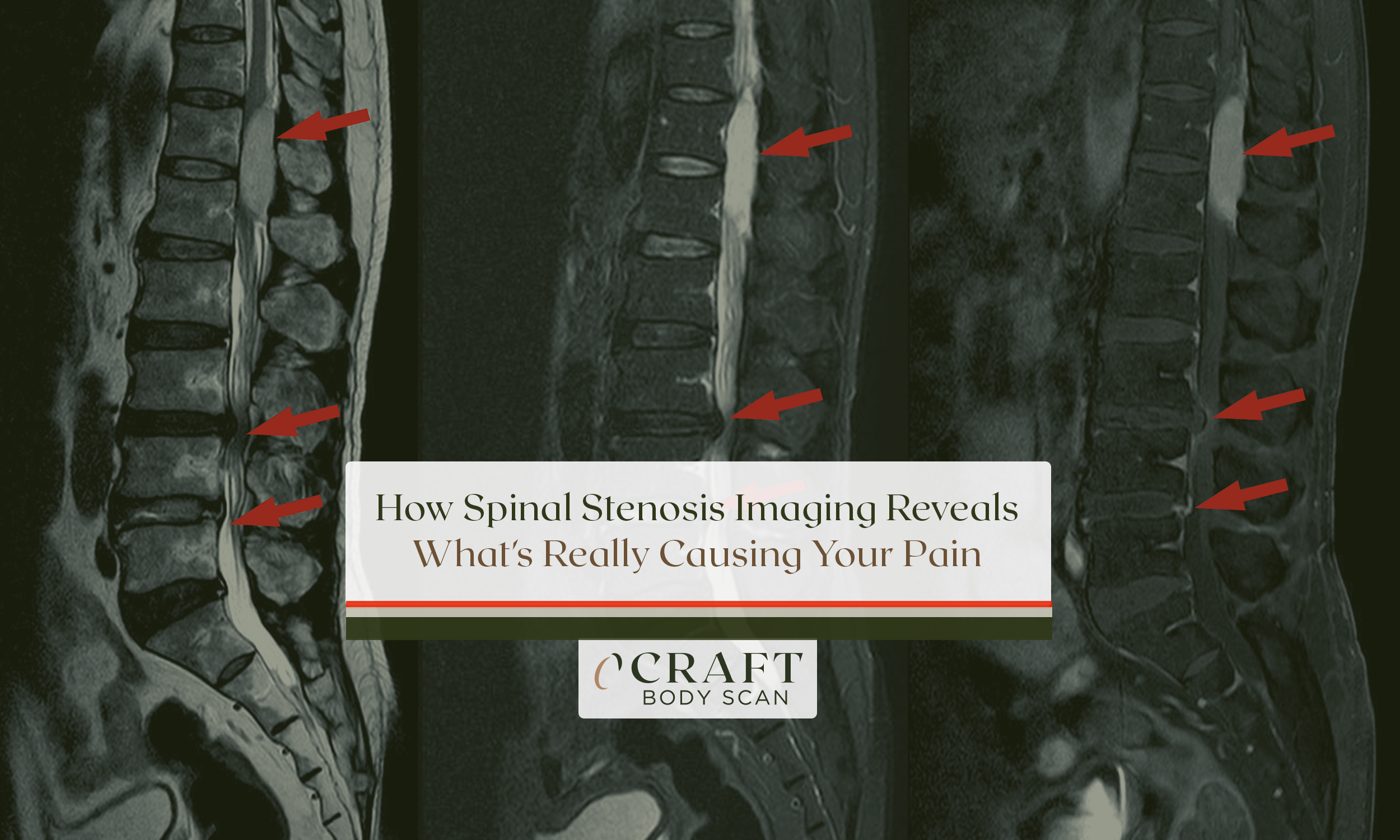
Stop guessing what’s happening inside your spine. Spinal stenosis imaging provides the definitive answer you need when back pain, leg numbness, or walking difficulties disrupt your daily life.
MRI and CT scans have transformed spinal stenosis from a mysterious condition diagnosed only through surgery into one that doctors can identify, measure, and treat with remarkable precision. For anyone over 50 experiencing symptoms that worsen with activity but improve when sitting or bending forward, these imaging technologies offer something invaluable: clarity.
Understanding What Spinal Stenosis Actually Does to Your Body

Your spinal canal houses and protects the most critical communication pathway in your body. When that canal narrows, the compression creates symptoms that can range from mildly annoying to completely debilitating. Spinal stenosis develops gradually, which explains why most people don’t notice anything wrong until their 50s or beyond. The condition affects approximately 103 million people worldwide who experience lumbar spinal stenosis alone.
The narrowing happens in three distinct zones. Central canal stenosis compresses the spinal cord or nerve bundle directly. Lateral recess stenosis affects the areas where nerve roots travel before exiting the spine. Foraminal stenosis occurs at the specific exit points where individual nerves leave the spinal column. Each type creates its own pattern of symptoms, and many people have multiple types simultaneously.
What causes the canal to narrow? In about 91% of cases, the answer is simply time and use. Your intervertebral discs lose height and bulge outward. The ligamentum flavum – a stabilizing ligament running along the back of your spinal canal – thickens and buckles inward. Facet joints develop arthritis and enlarge. Bone spurs form as your body attempts to stabilize segments that have become unstable. It’s not one dramatic injury but rather accumulated changes from decades of movement.
The location matters tremendously. Lumbar stenosis affects your lower back and compresses the cauda equina – the bundle of nerve roots below your spinal cord. This creates the classic pattern of leg pain, cramping, and numbness that worsens with walking but improves when you sit down or lean forward. Cervical stenosis occurs in your neck and can compress the actual spinal cord itself, potentially causing problems in all four limbs, balance difficulties, and fine motor challenges like trouble buttoning shirts or writing.
Why MRI Has Become the First Choice for Diagnosis
When your doctor suspects spinal stenosis, they’ll likely order an MRI first. This technology has several advantages that make it ideal for evaluating spinal canal narrowing. MRI visualizes soft tissues with exceptional clarity, shows the relationship between bones, discs, ligaments, and nerves in remarkable detail, requires no radiation exposure, and identifies spinal cord damage in cervical stenosis cases.
The examination itself takes 30 to 60 minutes. You’ll lie on a sliding table that moves you into a cylindrical scanner. The machine uses powerful magnets and radio waves to create cross-sectional images of your spine. Different sequences capture different tissue properties – some make fluid appear bright while others highlight inflammation or fat around compressed nerves.
What radiologists see on your MRI tells them exactly how severe your stenosis has become:
- Disc bulges and herniations – These show how intervertebral discs press against neural structures, narrowing the available space for your spinal cord or nerves.
- Ligamentum flavum thickening – This appears as a dark band encroaching on the bright cerebrospinal fluid that normally surrounds your nerves.
- Facet joint enlargement – Arthritic joints appear darker and bulkier than normal, contributing to canal narrowing from the sides.
- The “sedimentation sign” – In healthy spines, nerve roots settle to the back of the dural sac when you’re lying down. In severe stenosis, they remain clumped together, unable to separate.
- Spinal cord signal changes – For cervical stenosis, bright areas within the cord itself indicate myelopathy, where compression has damaged the cord tissue.
Doctors use standardized grading systems to ensure consistent diagnosis. The Lee grading system classifies central canal stenosis from grade 0 (normal) to grade 3 (severe). Grade 1 shows some cerebrospinal fluid around the nerve bundle but with reduced separation between rootlets. Grade 2 reveals no fluid between individual rootlets, though you can still distinguish them. Grade 3 indicates severe stenosis where the entire nerve bundle appears as a single mass with no visible separation.
These grades correlate with symptoms but don’t determine them. Some people with grade 3 stenosis experience minimal discomfort, while others with grade 2 find their quality of life severely affected. The imaging provides objective evidence, but your experience matters more than the numbers alone.
When CT Scanning Provides Information MRI Cannot

CT imaging delivers superior bone visualization compared to MRI, making it essential for surgical planning and for patients who cannot undergo MRI due to pacemakers or other implanted devices. The scanner uses X-rays to create detailed cross-sectional images in just 10 to 15 minutes – much faster than MRI.
CT excels at showing:
- Bone spurs (osteophytes) – The exact size, shape, and location of bony growths narrowing your spinal canal
- Calcified disc material – Hardened disc fragments that appear bright on CT but can be difficult to distinguish on MRI
- Facet joint changes – Detailed images of arthritic joint surfaces and how they contribute to narrowing
- Spinal canal dimensions – Precise measurements of the bony canal diameter and cross-sectional area
For complex cases, CT myelography combines contrast dye injection with CT scanning to achieve 94.4% sensitivity for detecting stenosis. This invasive but highly accurate test requires a lumbar puncture to inject contrast material into the spinal fluid. The contrast outlines your spinal cord and nerve roots, creating detailed images that show exactly where and how severely compression occurs.
Doctors order CT myelography when MRI proves inconclusive, when you have metal implants preventing MRI, or when multilevel disease makes determining which level causes your symptoms challenging. Research shows CT myelography identifies additional stenotic levels missed by standard MRI in 58% of multilevel cases.
Interestingly, CT and MRI measurements don’t always match perfectly. CT measurements typically show smaller canal cross-sectional areas than MRI – averaging 63.13 mm² versus 75.08 mm². This occurs because CT discriminates cortical bone better than MRI, leading to slightly different measurement boundaries. Both remain accurate; they simply measure slightly different aspects of canal anatomy.
How Your Imaging Results Determine Your Treatment Path

The most critical question isn’t what your imaging shows, but rather what that information means for your treatment. Spinal stenosis imaging guides the decision between conservative management and surgical intervention by revealing the severity of narrowing, the structures involved, and whether nerve damage has occurred.
Several imaging findings suggest conservative treatment will likely succeed:
- Mild to moderate stenosis – When adequate cerebrospinal fluid space remains around nerve roots
- Absence of cord signal changes – No bright areas within the spinal cord indicating tissue damage
- Stable alignment – No evidence of vertebral slippage or instability
- Minimal nerve compression – Nerve roots remain visible and separated rather than compressed together
Physical therapy produces outcomes comparable to surgery in many mild-to-moderate cases. Research shows 59% of patients receive physical therapy as first-line treatment, and those who begin within six weeks have reduced likelihood of needing surgery within a year. Conservative management includes targeted exercises that increase spinal stability, anti-inflammatory medications to reduce nerve irritation, epidural steroid injections for temporary relief, and activity modifications that minimize symptom triggers.
Other imaging findings may indicate surgery offers the best outcome:
- Severe central stenosis – Dural sac area measuring under 50 mm²
- Complete CSF obliteration – No visible fluid around the nerve bundle
- Cervical cord signal changes – Bright areas indicating myelopathy from cord compression
- Progressive neurological deficits – Worsening weakness or bowel/bladder dysfunction
- Spinal instability – Vertebral slippage (spondylolisthesis) occurring in 20-30% of stenosis cases
Surgical outcomes are generally favorable when appropriately selected. Between 70-80% of patients experience significant symptom improvement, with leg pain relief rates reaching 80-90% after decompression surgery. The procedure removes bone, ligament, and disc material compressing neural structures, creating more space for the spinal cord and nerves.
Imaging also helps rule out conditions that mimic stenosis but require entirely different treatment. Tumors pressing on the spinal cord, infections causing vertebral destruction, compression fractures from osteoporosis, and vascular claudication from arterial disease can all cause similar symptoms. Accurate imaging prevents misdiagnosis and ensures you receive appropriate care.
What to Expect During Your Spinal Imaging Appointment
Understanding the imaging process beforehand reduces anxiety and helps you prepare. For MRI, arrive 15-30 minutes early to complete safety screening forms. You’ll change into a hospital gown and remove all jewelry, watches, credit cards, and metal objects. The technologist will position you on a sliding table with padding and cushions for comfort.
Inside the scanner, you’ll hear loud tapping, thumping, and buzzing sounds as the machine creates images. Earplugs or headphones with music help mask the noise. The most important requirement is remaining still – any movement blurs the images and may require repeating sequences. A two-way intercom allows constant communication with the technologist, and a squeeze-ball lets you signal if you need to stop.
Claustrophobia affects approximately 12.5% of the population, but multiple solutions exist. Wide-bore MRI scanners with 70cm openings (versus standard 60cm) enable 99% of claustrophobic patients to successfully complete their scans. Open MRI systems with sides completely open provide alternatives for severe cases, though image resolution may be somewhat reduced.
Other strategies that help include oral anti-anxiety medication taken 30-60 minutes before the scan, deep breathing techniques and meditation during the examination, music through headphones to create a more pleasant experience, eye masks or closing your eyes to reduce visual awareness of the confined space, and having a family member present in the room when facility policy allows.
CT scanning presents fewer comfort challenges. The large, open design causes minimal claustrophobia, scans complete in 10-15 minutes, no loud noises occur during imaging, and you can communicate easily with the technologist throughout. However, CT uses ionizing radiation, making MRI preferable when both options provide adequate diagnostic information.
Advances Making Spinal Stenosis Diagnosis More Accurate
Artificial intelligence has transformed spinal imaging over the past two years. AI algorithms now achieve expert-level performance in detecting stenosis, measuring canal dimensions, and identifying subtle pathology that might escape initial notice. These systems analyze images automatically, grade stenosis severity using standardized scales, and flag concerning findings for radiologist review.
The practical benefits include shorter examination times (new AI-driven platforms cut MRI times by up to 60% while maintaining image quality), more consistent measurements across different readers and facilities, earlier detection of progressive narrowing on follow-up studies, and reduced radiation exposure during CT-guided procedures.
Three-dimensional reconstruction technology allows surgeons to visualize your specific anatomy before entering the operating room. They can plan the exact approach, anticipate challenges, and customize the procedure to your unique spinal structure. This preoperative planning contributes to better outcomes and reduced surgical time.
Take Control With Accurate Diagnosis

Spinal stenosis symptoms don’t have to remain a mystery. When walking becomes difficult, when leg pain forces you to stop and rest, when numbness or weakness affects your daily activities, imaging provides the answers you need to move forward with appropriate treatment.
The choice between conservative management and surgical intervention depends on correlating imaging findings with your specific symptoms and functional limitations. Some patients with moderate imaging findings will achieve excellent outcomes through physical therapy, anti-inflammatory medications, and activity modification. Others with similar imaging but progressive symptoms or failed conservative treatment will benefit from surgical decompression.
What matters most is having the diagnostic information necessary to make informed decisions about your care. Spinal stenosis imaging has evolved from a basic diagnostic tool into a precise roadmap that guides treatment selection, predicts likely outcomes, and helps you understand exactly what’s happening inside your spine.
Schedule your Craft Body Scan today and take the first step toward early detection and peace of mind. Our board-certified radiologists provide detailed imaging interpretation and clear explanations of your findings, giving you the knowledge needed to discuss treatment options confidently with your physician. Don’t let uncertainty keep you from the active, pain-free life you deserve.