The Prostate’s Core Functions in Men’s Health
 Your prostate may be small, but it performs several critical tasks that affect both fertility and daily comfort:
Your prostate may be small, but it performs several critical tasks that affect both fertility and daily comfort: - Produces seminal fluid: About 25-30% of semen comes from prostate fluid. This specialized liquid contains enzymes (including prostate-specific antigen or PSA), zinc, and citric acid that protect sperm and help them survive the journey through the reproductive tract.
- Powers ejaculation: When you orgasm, smooth muscle fibers in the prostate contract forcefully, pushing semen through the urethra and out of the penis. Without this muscular action, normal ejaculation wouldn’t be possible.
- Controls urine flow: The prostate wraps around part of your urethra – the tube that carries urine from the bladder. It functions like a valve, closing off the bladder during ejaculation to keep semen and urine separate, then opening to allow normal urination.
- Processes hormones: Inside the prostate, testosterone converts into dihydrotestosterone (DHT), a more potent hormone that influences prostate size and function throughout your life.
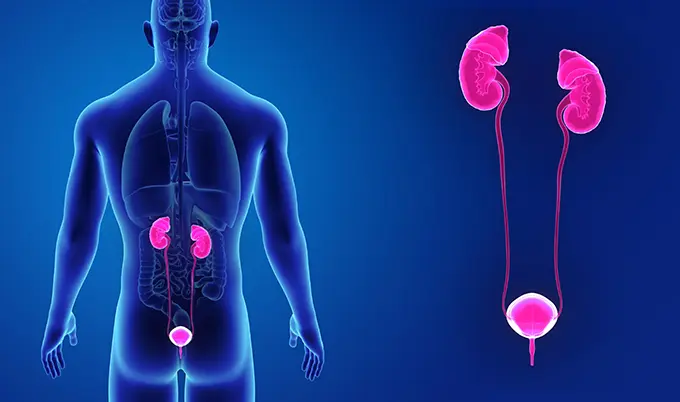
Where the Prostate Sits and Why Location Matters
The prostate’s location in your pelvis explains why problems with this gland affect multiple body functions:- Below your bladder – directly underneath where urine is stored
- In front of your rectum – which is why doctors can feel it during a digital rectal exam
- Surrounding your urethra – the tube that carries both urine and semen out of your body
The Prostate’s Three-Zone Structure
1. Transition Zone (10% of prostate tissue)
This innermost section wraps directly around your urethra and continues growing throughout life. It’s where benign prostatic hyperplasia (BPH) typically develops – the age-related enlargement that causes urinary symptoms in most older men.2. Central Zone (25% of prostate tissue)
Surrounding the transition zone, this area protects the ejaculatory ducts and contributes to seminal fluid production. Disease rarely affects this zone, making it the quietest section of your prostate.3. Peripheral Zone (70% of prostate tissue)
This largest section makes up most of your prostate’s mass and produces the majority of prostate fluid. About 70% of prostate cancers start here. Because it touches the rectum, doctors can feel abnormalities in this zone during exams.Common Conditions That Affect Prostate Function
 Three main conditions account for most prostate problems. Recognizing the differences helps you understand what might be happening and when to seek help.
Three main conditions account for most prostate problems. Recognizing the differences helps you understand what might be happening and when to seek help. “I like to tell patients that the prostate is kind of like an orange with a straw going right through the middle of it,” explains Dr. Scott Cheney, M.D. (Mayo Clinic Urologist). “And as we age, the prostate gets larger and larger, and the urethra gets compressed by the tissue of the prostate. This makes it more difficult for the bladder to push urine through the urethra, making it harder to empty the bladder.”
Quick Comparison: BPH vs Prostatitis vs Prostate Cancer
| Characteristic | BPH (Enlarged Prostate) | Prostatitis (Inflammation) | Prostate Cancer |
|---|---|---|---|
| How it develops | Gradual growth over years | Sudden or chronic inflammation | Slow cell growth (usually) |
| Pain level | Rare | Common, can be severe | Rare in early stages |
| Urination issues | Difficulty starting, weak stream | Painful burning sensation | Difficulty (late stages) |
| Age group | 50+ (90% of men over 80) | Any age | Typically 60+ (can start earlier) |
| Fever | No | Often present | No |
| Detection method | Physical exam, symptom assessment | Urine test, physical exam | PSA test, MRI, biopsy |
| Treatment approach | Lifestyle, medication, procedures | Antibiotics, pain management | Surgery, radiation, monitoring |
Warning Signs That Your Prostate Needs Attention
Most prostate problems develop gradually, but certain symptoms deserve immediate action. Here’s what to watch for: Common symptoms suggesting a prostate issue:- Needing to urinate more often, especially at night
- Difficulty starting urination or weak urine stream
- Feeling that your bladder isn’t completely empty
- Sudden, urgent need to urinate
- Pain or burning during urination
- Blood in urine or semen
- Painful ejaculation
- Discomfort in the pelvic area, lower back, or hips
Seek Immediate Medical Attention If You Experience:
- Complete inability to urinate – This is a medical emergency requiring urgent care
- Blood in urine with fever or chills – May indicate serious infection
- Severe pelvic or lower back pain – Especially if accompanied by urinary symptoms
- Painful urination with fever above 101°F (38.3°C) – Could signal acute prostatitis
Quick Assessment: Is Your Prostate at Risk?
Not everyone needs the same level of prostate monitoring. Use this assessment to see if early screening might benefit you.
Prostate Health Risk Factors
Check all that apply to you:
- Age 50 or older
- Black or African American (higher risk for prostate cancer)
- Father or brother diagnosed with prostate cancer
- Multiple family members with prostate cancer history
- Frequent nighttime urination (more than twice per night)
- Difficulty starting or stopping urination
- Weak urine flow or dribbling
- Feeling of incomplete bladder emptying
How Early Detection Changes Outcomes
Prostate cancer is the second most common cancer in men, but it’s also one of the most treatable when caught early. The five-year survival rate for localized prostate cancer approaches 100%.
The challenge? Early-stage prostate cancer rarely causes symptoms. By the time you notice urinary changes or discomfort, the disease may have progressed.
Traditional screening methods:
- PSA blood test: Measures prostate-specific antigen levels. Elevated PSA can indicate cancer, but also BPH or prostatitis
- Digital rectal exam (DRE): Doctor feels the outer portion of the prostate for lumps or abnormalities
While helpful, these methods have limitations. PSA levels can be elevated for non-cancerous reasons, and digital exams can only assess the peripheral zone (about 70% of the prostate).
| Age Range | Normal PSA Range | Screening Frequency |
|---|---|---|
| 40-49 years | 0 – 2.5 ng/mL | Establish baseline if high risk |
| 50-59 years | 0 – 3.5 ng/mL | Annual screening recommended |
| 60-69 years | 0 – 4.5 ng/mL | Annual screening recommended |
| 70+ years | 0 – 6.5 ng/mL | Every 2 years (discuss with doctor) |
Note: These ranges are general guidelines. Your doctor will consider your individual risk factors, symptoms, and medical history when interpreting PSA results.
Advanced MRI Screening for Comprehensive Prostate Health
Modern imaging technology has changed how we detect prostate problems. At Craft Body Scan, we use high-resolution MRI to provide detailed visualization that traditional screening can’t match.
Why MRI screening matters:
- Complete visualization: MRI images all three zones of the prostate, not just the outer surface
- Earlier detection: Can identify abnormalities before they elevate PSA levels
- Better accuracy: Helps distinguish between benign conditions and potential cancer
- Non-invasive: No radiation exposure, no need for biopsy unless truly necessary
- Comprehensive view: Shows surrounding tissues and can detect issues beyond just the prostate
Think of it this way: a PSA test is like checking your car’s “check engine” light – it tells you something might be wrong, but not what or where. An MRI is like opening the hood and actually seeing what’s happening inside.
For men with elevated PSA levels, family history, or concerning symptoms, MRI screening provides clarity that can guide better treatment decisions.
Schedule Your Prostate MRI Screening
When to Start Prostate Screenings
Timing matters when it comes to prostate screening. Current guidelines based on risk level:
High-Risk Groups (screening at age 40-45):
- Black or African American men
- Men with a father or brother diagnosed with prostate cancer before age 65
- Men with multiple family members affected by prostate cancer
- Men with known genetic mutations (BRCA1, BRCA2)
Average-Risk Men (screening at age 50):
- No family history of prostate cancer
- No known genetic risk factors
- Expected to live at least 10 more years
Consider earlier screening if you experience:
- Urinary symptoms that concern you
- Blood in urine or semen
- Erectile dysfunction that’s new or worsening
- Pelvic discomfort or pain
The decision to screen should be a conversation between you and your doctor, weighing your individual risk factors, values, and health goals. Our team at Craft Body Scan can help you understand your options and determine the right screening approach.
Lifestyle Factors That Support Prostate Function
While you can’t prevent all prostate problems, certain lifestyle choices may reduce your risk and support overall prostate health.
Diet: Foods That May Help
- Tomatoes and tomato products: High in lycopene, an antioxidant linked to prostate health
- Cruciferous vegetables: Broccoli, cauliflower, Brussels sprouts contain compounds that may protect cells
- Fatty fish: Salmon, sardines provide omega-3 fatty acids that reduce inflammation
- Green tea: Contains antioxidants that may support prostate health
- Limit red and processed meats: High consumption linked to increased prostate cancer risk
Physical Activity
- Aim for 150 minutes per week of moderate aerobic activity (brisk walking, swimming, cycling)
- Pelvic floor exercises (Kegels) may help with urinary control
- Maintain healthy weight: Obesity is linked to more aggressive forms of prostate cancer
- Stay active as you age: Regular exercise reduces BPH risk
Daily Habits
- Stay hydrated: Drink water throughout the day, but reduce fluids 2-3 hours before bed
- Limit caffeine and alcohol: Especially in the evening, as they can irritate the bladder
- Don’t smoke: Smoking is linked to more aggressive prostate cancer
- Manage stress: Chronic stress may worsen urinary symptoms
- Empty your bladder completely: Take your time urinating and don’t rush
Take Control of Your Prostate Health Today

Understanding what your prostate does – and what can go wrong – empowers you to take action before small problems become serious ones.
The prostate may be small, but its impact on your quality of life is significant. From reproductive function to daily comfort, this gland deserves your attention, especially as you age.
Key takeaways to remember:
- The prostate produces seminal fluid, controls urine flow, and helps with ejaculation
- Three main problems affect the prostate: BPH, prostatitis, and cancer
- Early detection dramatically improves outcomes for prostate cancer
- Advanced MRI screening provides more complete information than traditional methods
- Risk factors like age, race, and family history should guide your screening timeline
- Lifestyle changes can support long-term prostate health
At Craft Body Scan, we specialize in proactive health screening that detects potential issues before they cause symptoms. Our advanced MRI technology provides detailed insights into your prostate health, giving you the information you need to make confident decisions about your care.
Don’t wait for symptoms to tell you something’s wrong. Take a proactive approach to your prostate health with comprehensive screening.
Schedule Your Prostate Health Scan
Questions about prostate screening or MRI imaging? Contact our team to learn more about how we can help you stay ahead of potential health issues.
Frequently Asked Questions About Prostate Function
What happens if a man's prostate is removed?
If a man’s prostate is removed (prostatectomy) – typically to treat prostate cancer – he may experience changes in urinary and sexual function. Since the prostate helps control urine flow and produces part of the semen, common side effects include temporary urinary incontinence and dry orgasms (no ejaculation of fluid). However, with nerve-sparing surgical techniques, many men retain sexual function and regain bladder control over time. Recovery varies by individual and may involve physical therapy or medications to support healing.
Can you live without a prostate?
Yes, men can live full, active lives without a prostate. The gland can be surgically removed to treat prostate cancer or severe BPH. After removal, you can still urinate (though you may need time to regain full bladder control), and you can still achieve erections and orgasms. Natural fertility is affected since you’ll no longer produce the prostate fluid component of semen, but overall quality of life can remain high with proper medical care and recovery support.
What purpose does the prostate serve in the male body?
The prostate serves three main purposes: First, it produces about 25-30% of seminal fluid, which nourishes and protects sperm during ejaculation. Second, it helps control the flow of urine by surrounding part of the urethra and acting as a valve. Third, it processes hormones by converting testosterone into dihydrotestosterone (DHT), which influences prostate growth and function. These functions make the prostate essential for both reproductive health and daily urinary comfort.
What are the first signs of a bad prostate?
The most common early signs of prostate problems include needing to urinate more often (especially at night), difficulty starting urination, weak urine stream, feeling that your bladder isn’t empty after urinating, sudden urgent need to urinate, and pain or burning during urination. Some men also notice blood in urine or semen, painful ejaculation, or discomfort in the pelvic area. These symptoms can indicate BPH, prostatitis, or prostate cancer, so it’s important to consult a healthcare provider for proper evaluation.
Can you still get an erection without a prostate?
Yes, it’s possible to achieve and maintain erections after the prostate is removed, though it may be more difficult initially. Erections depend on the nerves and blood vessels surrounding the prostate, not the gland itself. If these nerves are preserved during surgery (nerve-sparing prostatectomy), many men regain erectile function over time – typically within 6-24 months. Some men may need medications, injections, or devices to support erectile function during recovery. Your individual outcome depends on factors like age, pre-surgery erectile function, and surgical technique.
What is the main cause of prostate enlargement?
The main cause of prostate enlargement (benign prostatic hyperplasia or BPH) is aging. As men get older, hormonal changes – especially shifts in testosterone and dihydrotestosterone (DHT) levels – cause the prostate gland to grow larger. This is a natural process that affects most men: about 50% of men in their 60s and 90% of men in their 80s have some degree of BPH. While BPH isn’t cancerous, it can cause urinary symptoms that affect quality of life. Family history, obesity, and certain health conditions may increase your risk.
How does the prostate affect urination?
The prostate surrounds the urethra – the tube that carries urine from your bladder out of your body. When the prostate is healthy and normal-sized, urine flows freely. However, when the prostate enlarges (as commonly happens with age), it can squeeze the urethra like a clamp on a garden hose, making it harder for urine to pass through. This causes symptoms like difficulty starting urination, weak stream, feeling of incomplete emptying, and frequent nighttime urination. The prostate also acts as a valve that closes off the bladder during ejaculation to prevent semen from mixing with urine.
At what age should I start worrying about my prostate?
Most men should start discussing prostate health with their doctor around age 50 if they’re at average risk. However, high-risk men – including Black men and those with a family history of prostate cancer – should begin conversations about screening at age 40-45. Even if you’re younger, pay attention to urinary symptoms like frequent nighttime urination, weak stream, or difficulty starting urination, as these can indicate prostate issues at any age. Early awareness and proactive screening give you the best chance of catching problems when they’re most treatable.